How to do Biometric Screening in 2024: The Complete Guide
How to do Biometric Screening in Worksite Wellbeing Programs
To better understand the importance of biometric screenings, I’ll tell you a short story. A while back my neighbor asked, “Will you look at my car? It is spewing white smoke.” He wanted to know what the problem was. You don’t have to be a mechanic to know that white smoke coming out of a car is a really bad thing.

It is a symptom of a much larger problem – in this case, a cracked engine block. The white smoke is caused by radiator fluid getting into the engine. This problem is fatal to the car and the only solution is a complete engine rebuild.
He was asked, “Did you notice the car acting funny?” He replied, “No, but a long time ago the check engine light came on.” He got tired of looking at the warning every day so he put a piece of black electrical tape over it, which made it a lot easier to ignore.
Had he taken his car to a mechanic, he would probably still have a functioning car today. The check engine light was an early warning signal that something was not quite right.
We all have early warning signals that come from our body when something is not quite right. We don’t get check engine lights; instead we get indications of high biometric values.
The biometric measures that come from our body can act as early warning signals that something is not quite right. If we ignore them, just like my neighbor ignored his check engine light, the odds of developing potentially fatal chronic diseases go way up.
Biometric screenings to determine these biometric measures (the “check engine” lights our bodies give us) are a foundational aspect of every successful wellness program. Regular biometric screenings allow individuals to identify early warning signals.
What Does a Biometric Screening Measure?
Among US adults, there are a lot of early warning signals coming from high blood pressure, high blood cholesterol and high blood glucose.
A government study looked at over 3,000 wellness programs and discovered that 62% of all wellness programs include biometric screenings. Among those same 3,000 programs, the following is a chart that shows the biometric measures that were included:
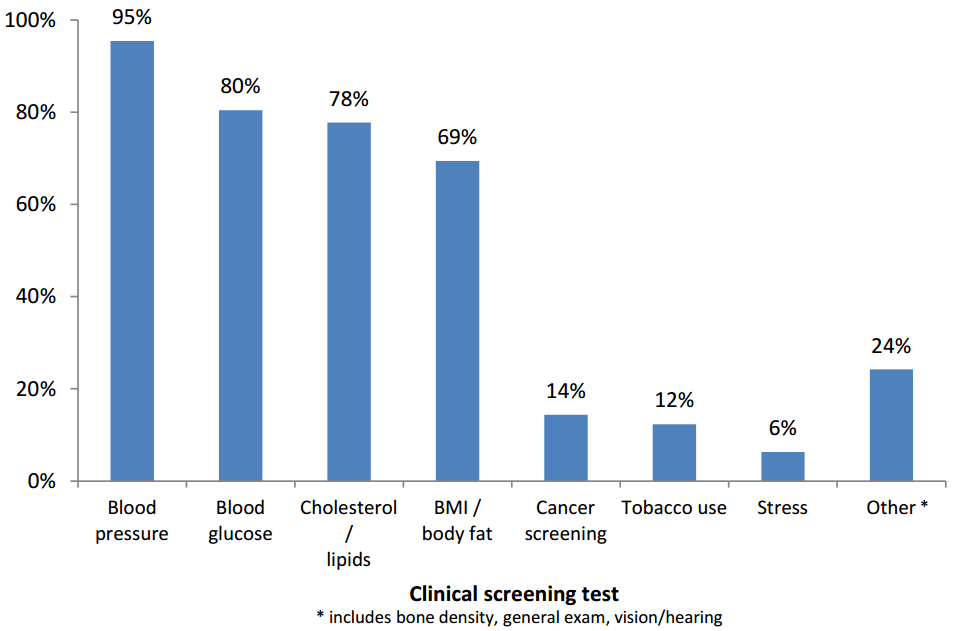
The primary measure workplace biometric screening programs are looking at is blood pressure, followed by blood glucose, blood lipids, and body mass index or body fat.
These four risk factors are the main focus of almost all screening programs. Increased competition and increased availability of screeners has made the cost of screening relatively low. It doesn’t take much to take a quick look at each of these four risk factors.
What are Healthy Biometric Values?
Blood Pressure:

Blood Glucose:

Blood Lipids:
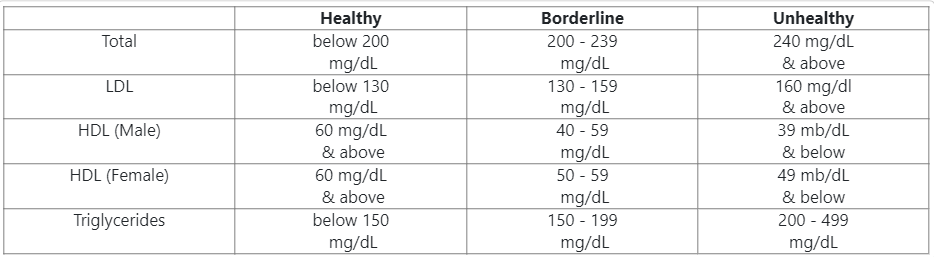
Body Mass Index (BMI):

Why Do Biometric Screening?
In the past 100 years, large epidemiological studies have shown us that elevated health risks are associated with the prevalence and incidence of the major chronic diseases.
All of these studies point to a very strong association between high levels of blood pressure, blood cholesterol, blood glucose, and body fat and chronic diseases such as heart disease, cancer, and diabetes.
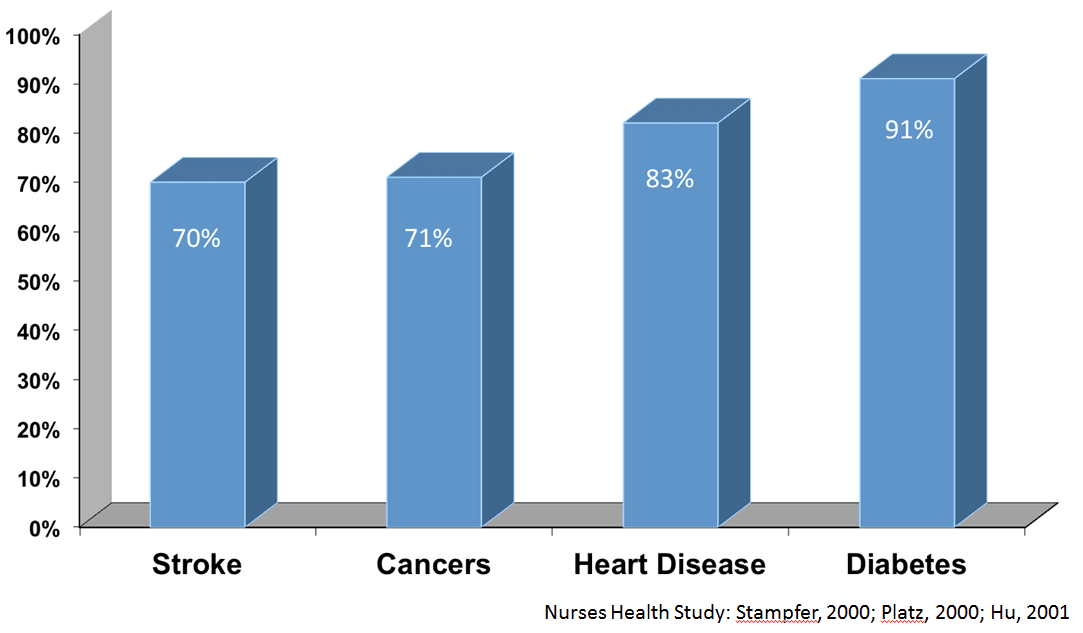
These connections between elevated health risks and chronic disease are very strong. During this same time frame, we have learned that if you can lower elevated health risks, chronic disease incidence also declines.
As Americans have worked to lower elevated health risks, the prevalence and incidence of heart disease has dropped substantially. Today heart disease death rates are lower than they have been in nearly 75 years.
The most recent data shows that for every 100 adults, 53 have elevated blood cholesterol, 33 have elevated blood pressure, and 10 are type II diabetic. Most adults in the United States have at least one elevated health risk and around half of them don’t even know it.
Finding people with elevated health risks and helping them adopt and maintain healthy behaviors is the key to lowering chronic disease prevalence and increasing the average life expectancy.
Wellness programs that can help individuals identify their health risks and improve their health behaviors by encouraging and providing biometric screenings will have a direct impact on the length and quality of life of their employees.

Biometric screening and intensive follow-up are probably the single most important thing wellness programs can do to improve employee health.
Despite the health advantages of having lower health risks, there is another reason why employers offer biometric screenings. Many employees like to track their own personal health. Biometric screening is like your own personal health dashboard.
Your own personal biometric data is a snapshot of your health. Elevated health risks can be predictors of future health and low health risks can be indicators of ideal health.
For many people, there is something inherently pleasurable about seeing low risk scores. Contrary to national recommendations, some people like to get their biometric values every year just because they can.
How to Do Biometric Screening
There are many options when it comes to gathering biometric data. If many of your employees are located in one geographical location, you might consider using an onsite biometric screening where a vendor comes in and gathers biometric data for all your employees at once. On-site screenings can cost between $45 and $70 per participant, but may require a minimum number of individuals.
If you have remote employees, multiple locations, or logistically cannot perform onsite screenings, your options include at-home testing kits, individual screenings with a primary care physician, or individual appointments at a third party screening facility.
Getting biometric data during a physician’s office visit generally costs between $100 and $200. It’s cheaper for groups that are self-insured to do screening on site.
However, if your organization is fully insured, employees can get their biometric data measured for free as part of their preventative services (which are now covered by most health plans). Take-home biometric screening kits cost between $40 and $50 each.

Besides the actual biometric screening cost, there are other costs that employers need to know about. Encouraging employees to do a biometric screening will cause some employees to have a physician’s visit and possibly start taking medications. That office visit and those new medications are additional costs that can add up.
I am currently involved in an analysis of the pharmaceutical costs for a wellness program. Early evaluations suggest that employees who do biometric screenings have higher pharmaceutical costs than those who do not.
This is to be expected, since the most common medical treatment for elevated health risks is medication. Biometric screening is the right thing to do to prevent chronic diseases and early death, but workplaces should realize that with all preventative services there is an associated cost. However, this initial cost will likely be significantly less than the cost of disease management if the problem being treated by medication is left unchecked.
There are a lot of good options to get screening work done. The bigger challenge is to organize and track the screening data you collect.
WellSteps has experience helping employer groups do this in a variety of different ways. On-site screeners can generally provide an Excel file of all biometric data, since WellSteps is a third party vendor. Over the years, WellSteps has used a variety of partners to conduct biometric screenings. Acquisitions and mergers within the industry have influenced both the price and quality of the screenings. WellSteps currently uses eHealthscreenings.com, but we are always reevaluating our vendors to make sure we use the best in the industry
Individual employees who get their biometric data from a kit or their personal physician can email or fax a copy of their results. One of the quickest and easiest ways for wellness programs to receive biometric screening results from individual employees is to use the WellSteps app.
Employees open the app and take a picture of their biometric screening form, which is automatically uploaded to a secure file. The WellSteps staff then verifies that the information is complete and uploads the biometric values so that it integrates with the WellSteps Personal Health Assessment data.
Just about everybody has a smart phone, which means that just about everybody has a way to very quickly and easily verify that they’ve completed their biometric screening.
How Often Should Employees Get Screened?
There are two ways to answer this question. They both depend upon the goals, objectives, and budget of your wellness program. The most effective and cost-effective way to screen employees is to follow the professional guidelines established by the U.S. Preventative Services Task Force. These guidelines when it is appropriate to get screened based on age, gender, and the presence of risk factors. These guidelines are not perfect, so they will and do change–but at the moment, they are the best we have.
It is NOT recommended that an entire employee population be screened every year.
Relative to other wellness interventions, screening is often very costly. The cost of annually screening every employee is always greater than any possible savings that might come from reduced chronic disease incidence or premature death. This approach makes the economics of mass biometric screening very dubious.

For example, if you screen for a risk that is present in 10 out of 100 people, you have to screen all 100 people just to find that 10 individuals who have elevated risk.
Then you have to help these 10 at-risk individuals adopt and maintain healthy lifestyles for the rest of their lives. And, if all goes well, some of these 10 people will avoid chronic diseases they would have otherwise developed.
In the table below is summarized the screening intervals that are recommended for blood pressure, glucose, and cholesterol. Based on the hundreds of research studies that are reviewed by the Preventative Services Task Force, these are the current recommendations that try to strike a balance between the cost of screening and the possible reductions in chronic disease incidence and prevalence.
| Risk Factor | Screening Interval |
|---|---|
| Hypertension | The optimal interval for screening adults for hypertension is not known. The Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7) recommends:
● Screening every 2 years with BP <120/80. ● Screening every year with SBP of 120-139 mmHg or DBP of 80-90 mmHg |
| Diabetes (glucose) | The first step should be measurement of blood pressure (BP). Adults with treated or untreated BP >135/80 mm Hg should be screened for diabetes. The optimal screening interval is not known. The ADA, on the basis of expert opinion, recommends an interval of every 3 years. |
| Hypercholesterolemia | The optimal interval for screening is uncertain. Reasonable options include every 5 years, shorter intervals for people who have lipid levels close to those warranting therapy, and longer intervals for those not at increased risk who have had repeatedly normal lipid levels.
An age at which to stop screening has not been established. Screening may be appropriate in older people who have never been screened; repeated screening is less important in older people because lipid levels are less likely to increase after age 65 years. |
Most workplaces either don’t know about these recommendations or don’t care. That is unfortunate, because they represent an enormous amount of careful research, consideration, and recommendations by an independent panel of professionals! These recommendations are the best information we have on how often to conduct screenings.
Despite these recommendations, WellSteps has worked with clients in the past who insisted that their employees be screened every year. They ignored the scientific guidelines because their employees liked to track their own biometric data.
An example is the CEO of a large construction company who had monitored his biometric scores for each of the last 15 years. His cholesterol levels, glucose levels, and blood pressures had fluctuated a little bit each year, but were essentially straight horizontal trend lines across the entire 15-year period. He was proud of the fact that little had changed in 15 years, even though one of his risk factors was borderline high during that entire time.
Certainly the fact that he had not gotten worse was good news, but the point is that some people just like to see their own data. Unfortunately, some of these people are decision-makers, who think everyone should be as data-driven as they are. Tracking and monitoring the data will not always lead to a change in behaviors, as much as we might like it to!
The U.S. Preventive Service screening recommendations say that doing biometric screening every year is not a smart use of time and money. Theses recommendations come from the best and brightest among us.
You can be armed with this knowledge and speak the truth until you’re blue in the face, even outlining how much money could be saved. But if employees love getting biometric data each year, you’re swimming uphill.
The bottom line is, if the act of getting screened is mentally associated with a monthly reduction in healthcare insurance premium, you’re out of luck.
In one example, all the employees who wanted the healthcare premium reduction had to complete the biometric screening and each year many of the employees were excited to share the results with fellow employees. The act of screening itself had become part of the workplace culture and was immoveable.
Despite the cost savings that could have been realized following the recommendations, they continued to do the annual screening. In their eyes, there was more value in the screening process than there was in actual savings associated with following national recommendations. Annual screening had become a ritual within this organization that everyone looked forward to and actually enjoyed.
After hearing their arguments, it became clear that the second answer to the question, “How often should employees get screened?” was as often as you like. This particular group has been doing annual biometric screening for over five years and, to them, the extra cost of the screening was worth it.
So there are really two answers to the “How often” question: 1) follow established biometric screening science so you can optimize your wellness dollars OR 2) throw the science to the wind and let your employees engage in an annual biometric screening ritual so long as you have the budget for it. And neither one would be wrong.
Biometric Screening is Easy. It’s What Comes Next That Matters
Despite what actually happens in many wellness programs, there are actually two important parts of having a successful biometric screening program. The first part is gathering data (bloodwork and measurements) and generating risk scores. This is the easy part. In fact, it’s so easy you can buy a kit and do it yourself at home. There are also medical professionals or vendors who are professionally trained to take your blood and calculate your results. The hard part is knowing what to do with the information once you have it.
Lowering elevated blood pressure, glucose, or cholesterol–now that is a different issue altogether. At the end of the day, isn’t that the reason for the screening in the first place? Doesn’t this whole situation reminds you of a Seinfeld sketch where Jerry talks about the difference between taking a car reservation and actually holding the reservation?
Typically, an employee who has recently received their biometric data will get a chance to visit with a nurse or a health coach. The results will be discussed and some recommendations will be made and, most likely, the employee will walk away with a brochure and encouragement to visit with a primary care provider.
This is all well and good and maybe even helpful, but this is also where the process breaks down. Employees with dramatically elevated health risks should be vigorously encouraged to seek medical attention.
The proper medical treatment protocol for elevated cholesterol and blood pressure is to first start with Therapeutic Lifestyle Change (TLC). This is a fancy way of saying adopting and maintaining a healthy lifestyle.
This is the correct approach to take with elevated health risks because, after all, the elevated health risks are almost always just a symptom of a larger problem: unhealthy behaviors.
If individual employees with elevated health risks adopt and maintain habits that include good nutrition and regular physical activity, meaningful improvements in their health risks will occur.
Despite this treatment protocol, most physicians are only able to provide some encouraging conversation and perhaps another brochure.

There are very few options to engage in therapeutic lifestyle change within the current medical community. Doctors are not reimbursed to have conversations with their patients.
They get paid when they put something in you or to take something out of you. Many doctors don’t ever talk about healthy lifestyles with their patients because they don’t believe patients will do anything anyway.
Why waste time talking about good nutrition and physical activity if the patient is unlikely to make the necessary behavior changes? Often, they are quick to prescribe risk-reducing medications. These medications work, but they don’t address the underlying problem of unhealthy behaviors.
To help employees with elevated health risks, wellness programs need to offer programming that is based on effective behavior change concepts. These can be challenges, campaigns, courses, or coaching sessions designed to help employees and their significant others improve nutrition habits, exercise patterns, sleep schedules, and mental health practices.
WellSteps does this by offering specific behavior change campaigns, challenges and WellSteps TLC. This program is effective at reducing elevated cholesterol, blood pressure, blood glucose, and body fat without medication.
If employees have high health risks after multiple attempts and considerable efforts to adopt healthy behaviors, then it’s time to start taking risk reducing medications.
Why It Is Hard to Lower Health Risks
Even with effective programming, it is hard for most people to lower their health risks. Besides the usual suspects–fast food, large serving sizes, processed foods, and sugar–there are other factors working against employees who have elevated health risks.
On average, as you age each year, blood pressure, cholesterol, and glucose values increase.

After age 30, cholesterol values increase in females about 3 mg/ml per year and in males about 1 mg/ml per year. After age 30, males and females will see blood pressure increase 1 mm/HG every year. Blood glucose does the same thing. After age 30, most adults will experience an increase in blood glucose of about 1 mg/ml per year.
This means that with the passage of time, employees who were once low risk will eventually become high risk. It also means that individuals who are high risk will get even higher. In ten years time, many healthy employees will have acquired elevated health risks.
For most people, elevated risks are elevated to a high-risk level because of unhealthy lifestyles. The elevated risks are the result of a physical reaction to unhealthy behaviors. Genetic causes of elevated blood pressure are very real, but not as strong as behavioral factors; genetic causes of high blood cholesterol are extremely rare – present in less than 1 percent of the population.
There is a natural flow of risk or, as the academics like to call it, natural risk migration that occurs each year. The complicated figure below shows how this works. Among a typical group of employees there will be some who have low risk, some who have moderate risk, and some who have high risk.
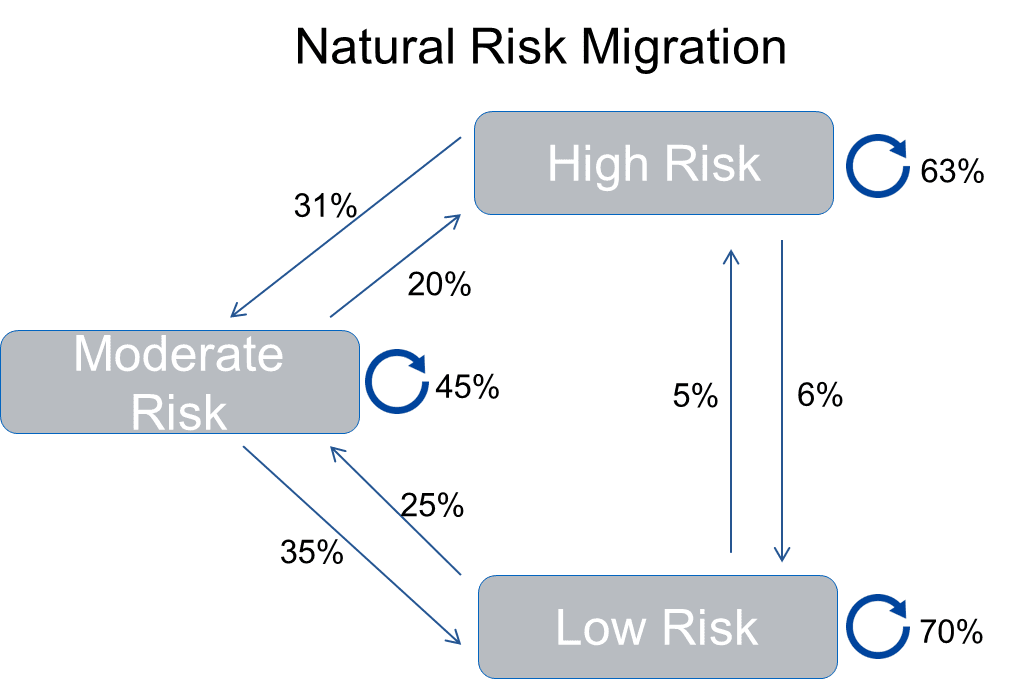
In just one year, many employees will move from one group to the other. Take, for example, the employees who are low risk at the beginning of the year. In 12 months, 70% of those employees will still be in the low risk category, 5% will migrate from low risk to high risk, and another 25% will migrate from low risk to moderate risk.
Even though they did not participate in any wellness programs or any intervention whatsoever, there will be a natural flow between risk levels. Most employees who have moderate risk at baseline stay there, but 20% move to high risk and 35% become low risk. In the high risk group most of them stay high risk after 12 months, with 6% moving to the low risk group and another 31% moving to moderate risk. This movement reflects changes in health risks that occur naturally.
Every wellness program must consider the natural risk migration that occurs among their employees. To document that a wellness program is having any effect on elevated health risks, your risk migration needs to be better than the natural risk migration that occurs.
With natural risk migration, it is possible that 6% of your high risk population may have become low risk, even if your program didn’t do anything. Be careful not to claim credit for changing employee health risks when similar changes can occur naturally.
Researchers, myself included, spend a lot of time looking at the impact of wellness programs. We are extremely careful to document that the programs do indeed change risk in ways that are significantly greater than natural risk migration.
Biometric Data Security
When personal health information is collected, all HIPAA privacy, security, and breach rules must be followed. Privacy policies on collection, storage, and disclosure must be provided and a third party must be used to analyze data. If you have questions on the compliance of your wellness program, use the free compliance checker tool here.
Putting It All Together:
Biometric screening and subsequent behavior change are some of the most rewarding aspects of employee wellness programs. This is where we save and transform lives. We have a good time and do fun activities, but, at the end of the day, it’s about improving the length and quality of people’s lives.
Good wellness programs save lives by focusing on behavior change that can make a big difference in health risks. Here is the typical process we take to help employees lower their health risks:
Get the Word Out
We have used the Know Your Numbers campaign to communicate, educate and motivate employees to get screened. We use the best marketing and messaging possible to persuade people that getting screened is a good idea.
Once everyone has been screened and their biometric data has been integrated with their personal health record, employees can see what risks they have. It works best when the employer group includes a meaningful incentive
One employee who completed the Know Your Numbers campaign said,
“This campaign made me aware that my blood pressure had changed, and I have taken the steps to get it back to normal.”
User stories like this are what wellness programs and employee biometric screenings are all about!
Include Everyone

One approach to helping employees change behaviors is to focus only on those employees who have elevated health risks. This is a pretty good strategy to take because you’re focusing on the worst cases first. However, natural risk migration tells us that with the passage of time most people will eventually develop elevated health risks.
You can focus on those employees who have elevated health risks and help them improve behaviors, or you can take a step back and consider offering behavior change interventions to every employee, including those with low health risks. This makes sense for several reasons:
As people age their health risks will increase and, eventually, more and more of your employees will develop elevated health risks. Also, by offering behavior change campaigns to all your employees at the same time you can capitalize on the group effect. The group effect happens when a large group of employees are simultaneously engaged in a single cause.
There’s always a sense of competition, camaraderie, and peer pressure that helps individuals have more success as a group than as individuals. WellSteps prefers to include all employees in behavior change campaigns and challenges, regardless of their health risks.
To help people lower blood cholesterol they should eat more vegetables. Getting the entire workforce to participate in the Veggie Up campaign means that all the employees are improving their vegetable consumption at the same time.
Again, targeting those with health risks is not a bad strategy, but we have found that including everyone in the adoption and maintenance of healthy behaviors has a more comprehensive and lasting impact.
Using this exact approach, we have published a variety of research studies documenting changes in employee health risks. The table below shows the changes in biometric health risks over a one year period among the 3500 employees of Boise School District. To get employees to participate, they were offered a $40 reduction in their monthly health insurance premium.
These results are typical of what we’ve seen for large groups of employees participating in a variety of behavior change campaigns. The results are favorable, but still not as good as when we use TLC. Here is the full paper that describes this program in more detail.
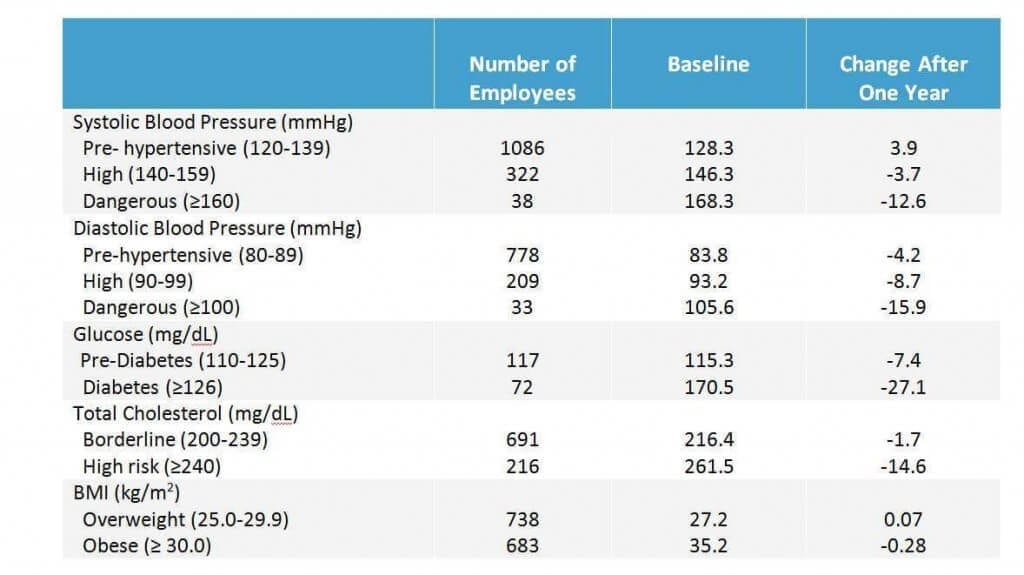
Boise School District is not the only workplace that has been able to produce results like this.
Many studies that show that aggressive behavior change programs both in the community and in workplaces can reduce elevated health risks in as little as six weeks. Even better results are seen at 6, 12, and 18 months.
Every year the Koop Award is given out to the best wellness programs in the United States. Almost without exception, every one of these programs has been able to demonstrate dramatic improvements in health risks.
Bring Out the Big Guns
The hardest thing for people to do is to change behaviors. Elevated blood cholesterol, blood pressure, and blood glucose doesn’t just happen overnight -these elevated health risks developed over decades of an unhealthy lifestyle. Since it takes decades to develop these elevated health risks and the habits that precede them, reversing the process can be difficult.
For many employees, participation in some targeted behavior change campaigns and challenges will make a difference, but for others a more aggressive approach is required.
This is why WellSteps has developed WellSteps TLC. WellSteps TLC is a lifestyle change program that consists of extensive behavior change programming specifically targeting nutrition and physical activity.
It includes all of the education, tools, strategies, motivation, and support from others that individuals need to successfully adopt healthy behaviors. It is a clinically backed program that teaches and encourages changes in nutrition and physical activity that result in lower employee health risks.
For example, employees with elevated blood cholesterol benefit greatly from TLC. Employees who will decrease their saturated fat to less than 7% of total calories can reduce their LDL-cholesterol by 10%. Here’s what the research shows about the impact of TLC.

Each TLC module includes a video, behavior change tasks, social support, and gamification. Participants can participate via computer or using any mobile device. Each module is interactive and participants must complete simple behavior change tasks before they can progress to the next module.
Each time employees participate, they can interact with others who are working through the same lifestyle transformation. The program includes healthy recipes, cooking and grocery shopping ideas, and discussions from behavior change experts.
After participating in TLC, if an individual still has elevated health risks it’s time to visit with a healthcare provider about starting a regimen of risk-reducing medications.
Medications are effective at reducing elevated health risks and they have the ability to reduce the prevalence of chronic diseases. TLC is the first step that everyone should take to improve their health, but if those efforts fail it’s time for employees and their spouses to work with their healthcare provider to get more aggressive treatment.
So What Next?
If the goal of your wellness program is to improve employee health and reduce healthcare costs, then helping your employees complete a biometric screening and behavior change program are a must.
Done right, biometric screening and subsequent behavior change programming will likely be the most effective part of your wellness efforts.
Any wellness program that can document significant reductions in elevated health risks is well on its way to reaching its wellness goals. Improving health risks is also a good indicator that the wellness program has been properly designed and executed. Schedule a free demo with our team today to know the next steps in getting started!







