Executive Summary
How do corporate employee wellness programs save companies money?
Corporate employee wellness programs save money by reducing preventable healthcare costs, lowering absenteeism, and decreasing employee turnover. Healthier employees use fewer medical services over time and miss fewer workdays due to illness or injury. Well-designed programs also improve productivity and retention, which reduces the high costs of recruiting, hiring, and training new employees.
What should I know about the worksite?
For three years, a school district implemented comprehensive employee wellness programs and saw many benefits. This blog summarizes research showing that the school district reduced elevated health risks and lowered medical costs.
It is based entirely on peer-reviewed, scientific evidence, and you’ll discover how similar programs can benefit your company as well.
For the three years prior to the implementation of a worksite wellness strategy, (between 2009 and 2011), the 3,269 employees of a large school district in the Rocky Mountain area experienced total medical costs of between $11,000,000 and $13,000,000 per year. Equally sized employers in the Western U.S. experienced similar health care cost trends.
During this time period:
- 60 percent of district employees suffered from having higher weight or obesity
- 61 percent had hypertension or prehypertension
- 39 percent had high or borderline high cholesterol
- 5 percent had diabetes or pre-diabetes
- average age was 50
- approximately 15% of employees worked in manual occupations
Local taxes funded the district’s health care costs. The district was, and continues to be, fully insured with a retained-retention agreement that gives their medical plan the benefits of a self-funded health plan. As a result, the district receives any health care premium payments that exceed actual health care costs.
A stop-loss policy reinsures claims costs above $250,000. The combination of poor health behaviors, elevated health risks and increasing medical cost trends convinced the district to begin a comprehensive worksite wellness strategy.

RELATED: 9 Reasons School Wellness Programs Are a Smart School Strategy
What should I know about their corporate employee wellness program?
The district hired a full-time worksite wellness program coordinator and selected WellSteps as its wellness vendor. The wellness program design rested on the premise that poor employee health strongly influences absenteeism, presenteeism, and medical costs.
Elevated health risks—most of which stem from poor lifestyle choices—directly cause poor health. Therefore, to impact employee-related expenses, wellness programming focused on the root cause of poor health ─ unhealthy behaviors.
Elevated health risks—most of which stem from poor lifestyle choices—directly cause poor health.
The district designed its wellness program to help employees improve health behaviors and create a work culture that supports healthy practices. The program provided employees with the education, awareness, motivation, tools, strategies, supportive policies, and social support needed to adopt and maintain healthy behaviors as scientifically well-documented by Dr. Michael O’Donnell.
Gathering Data
Before participating in the program, employees completed a self-reported Personal Health Assessment (PHA) after which they received individualized electronic feedback. Additionally, to assess health-promoting policies and environments, the onsite wellness program coordinator and some committee members completed a health culture audit called “The Checklist to Change.”
RELATED: Checklist to Change Personalized Audit Questionnaire
A WellSteps account manager summarized and discussed data from the PHA and Checklist to Change with the onsite wellness coordinator. As an illustration, figure 1 shows the components used to design the overall wellness strategy.
The program incorporated administrative planning, baseline data evaluation, culture change and communication strategy, biometric screening, behavior change campaigns, and more. The district offered four campaigns each year, each lasting four to eight weeks.
Behavior Change Campaigns are unique to WellSteps. The campaigns improve health behaviors and build self-efficacy by breaking behavior change into manageable weekly tasks.
RELATED: How to do Biometric Screenings: The Complete Guide
How do health and wellness incentives influence outcomes?
Two types of incentives were used to promote program participation. Those who completed behavior change campaigns were entered into a drawing for gift cards to local retail stores. A second, more robust incentive was benefits-based. These were changed each year and are described in Table 1.
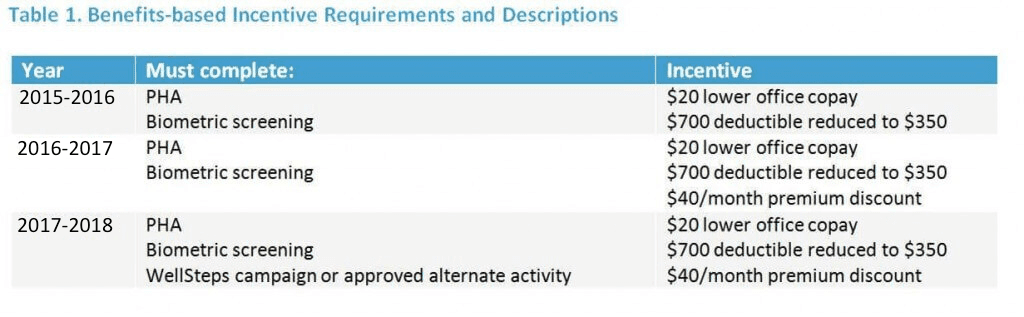
RELATED: Wellness Program Incentives: The Complete Guide
What results can corporate employee wellness programs produce?
The WellSteps model that was used suggested that improved health behaviors would lead to lower health risks and subsequent reductions in medical costs. As has been noted in peer-reviewed scientific papers documenting the effectiveness of the model in this district, which have been previously published here and here.
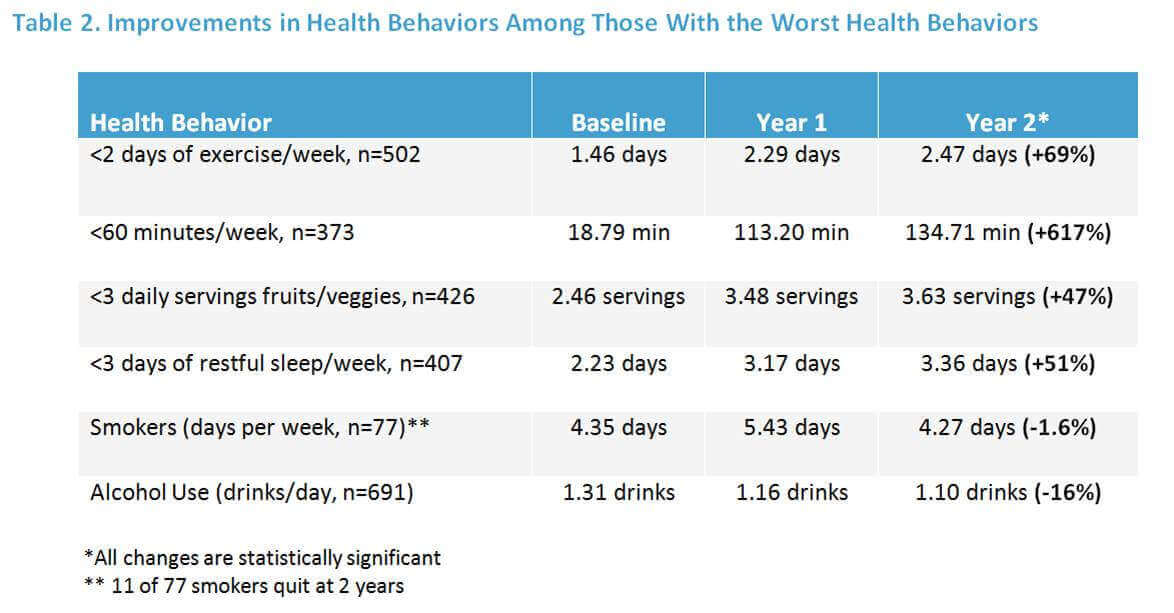
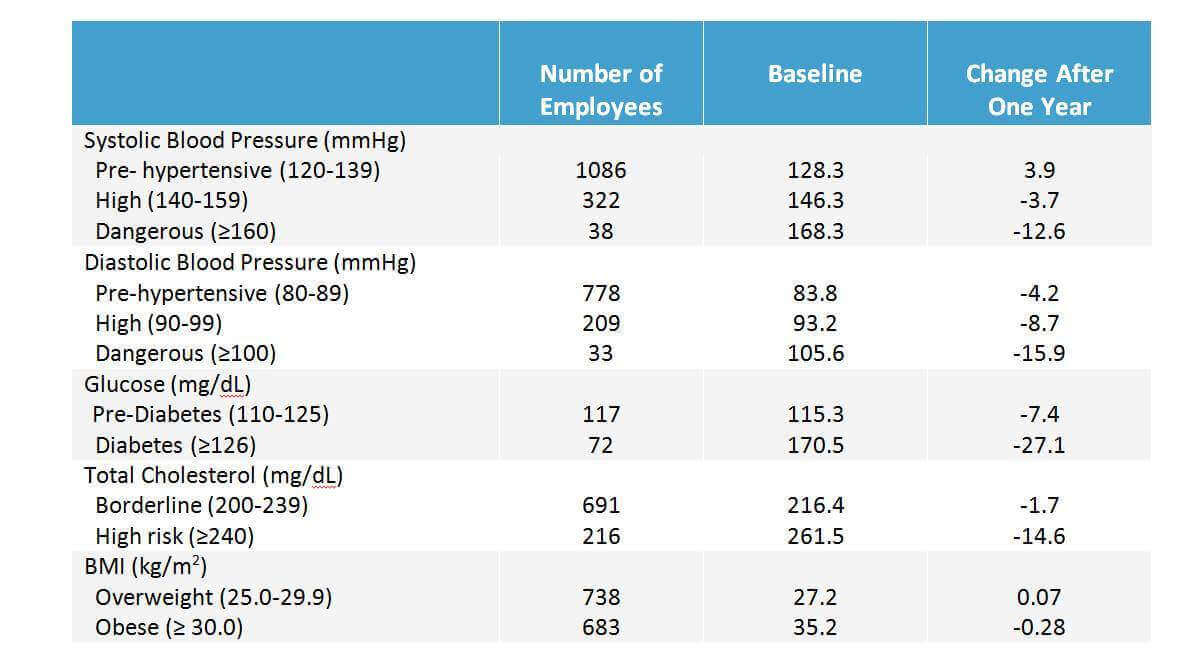
Table 2 shows improvements in nutrition, physical activity, tobacco, and alcohol use among those with the unhealthiest baseline behaviors. These behaviors improved from baseline and continued improving through at least two full years. Table 3 shows changes in biometric health risks. There was consistent risk reduction among those who had the unhealthiest numbers at baseline.
RELATED: Employee Health Programs Worth Investing In
Did this wellness program save money?
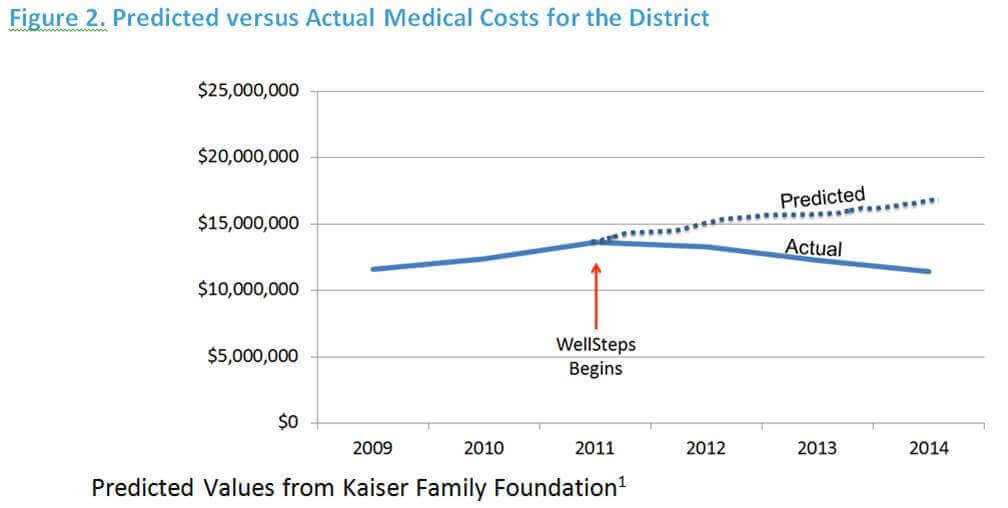
Figure 2 below shows the predicted medical costs if the district had followed the same cost trends of comparable worksites. This prediction provides a good estimate of what the cost trend would have been in the absence of a wellness program.
However, the district did not experience the predicted trend of comparable worksites. Rather, district medical costs peaked in 2011, then decreased each year through the end of the evaluation period (2014). The district medical costs in 2014 ($11,390,481) were lower than the costs in 2009 ($11,590,407). Basically showing a zero trend across the six-year evaluation period.
Individual wellness program participation data were then combined with individual medical cost data to allow for comparison of the medical costs between wellness program participants and non-participants. Six years of medical cost data were evaluated, including the three years prior to wellness program implementation.
The Results
In short, the “pre-program” cost data was used to statistically remove pre-existing differences in cost between participants and non-participants. During the three-years prior, program non-participants had slightly higher medical costs ($3,414 vs $3,308). No differences existed in age or sex between participants and non-participants.
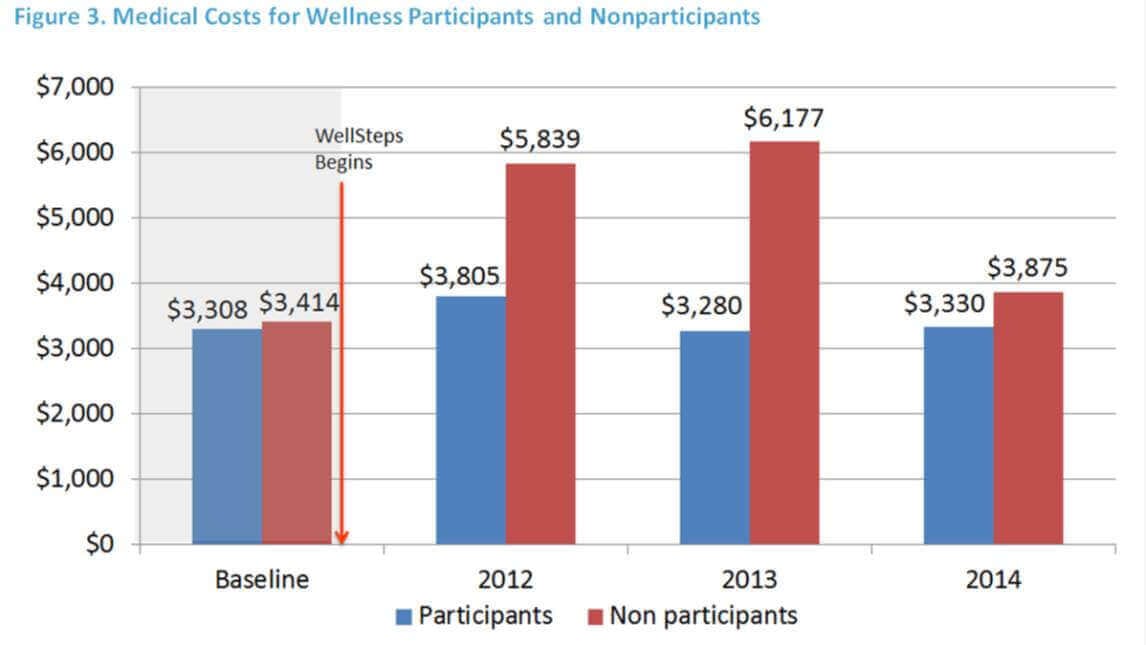
Post-implementation, there was, furthermore, a dramatic difference in the cost of medical care between the employees who participated in the wellness program and non-participants in 2012 and 2013, and to a lesser extent in 2014 (Figure 3).
During the three-year period starting with 2012 and ending with 2014, the program participants cost the district $5,025,138 less in medical costs than non-participants. Because the impact of other variables was statistically removed, it is highly likely that this cost savings is primarily due to the impact of the comprehensive wellness program.
The cost of providing the wellness program during the same three-year period was $1,412,736. Thus, the benefit-to-cost ratio for the program was 3.56 ($5,025,138/$1,412,736). During this study there were no changes in the district’s health plan design.
RELATED: Wellness ROI vs VOI: The Best Employee Well-Being Ideas Use Both
What limitations should employers consider in wellness programs?
Despite the improvements in health behaviors and risks, BMI did not improve. But while the U.S. population as a whole grew heavier during the three years under evaluation, the participants in this study did not. So, while there was no loss of weight, participants did not gain weight either.
What key lessons can employers learn from wellness program outcomes?
Randomized clinical trials (RCTs) are an evaluation gold standard and none of the studies on which this report is based were (RCTs). However, it is currently illegal to randomize employees to a non-wellness program condition.
This criticism aside, we ask: If the worksite wellness program was not responsible for these documented improvements in health behaviors, health risks, and medical costs, than what was? These findings show the published research that answers the question, do wellness programs save money?
A worksite with a zero medical cost trend over a six-year period is extremely rare. This paper provides ample evidence to show that worksite wellness strategies can be effective at promoting health and reducing employee medical expenses.
In summary, this paper provides ample evidence to show that worksite wellness strategies can be effective. Effective at both promoting health and reducing employee medical expenses.
Note: the health care cost findings in this blog were previously published in the journal Preventive Medicine.
Frequently Asked Questions
An employee wellness program, in general, is any worksite activity designed to support better employee health. These activities often include medical screenings, incentives for healthy behaviors, behavior change interventions, health coaching, fitness, nutrition, and weight loss programs, social support, gamified wellness challenges, and much more.
Employees are not mere economic units. The entire spectrum of human well-being plays into how well an employee feels and performs at their job. For this reason, a good employee wellness program must take into consideration the following:
physical wellness
mental wellness
emotional wellness
social wellness
financial wellness
A well-organized employee wellness program can produce important outcomes. Outcomes such as improved employee health behaviors, lower health risks, and reduced health care costs. They are also effective at improving employee morale and productivity.
Employee wellness programs are effective when they include tailored recommendations, an interactive platform, simple tracking, engaging challenges, and meaningful incentives. Put simply, give great resources, engaging content, and motivating incentives to ensure success. All of these elements come together on the WellSteps Wellness Platform (https://www.wellsteps.com).
Employee wellness programs support better health outcomes by giving employees consistent, structured ways to improve daily habits. Building on good habits and replacing poor habits leads to consistent improvements toward a happier, healthier individual. Wellness programs with customized offerings and recommendations encourage users to seek preventative screenings, set goals, act daily, and increase healthy habits through engaging tools and content.
Companies keep participation high by offering in many ways. One of the best ways to keep engagement up is to watch the data and talk to the participants. Data doesn’t lie. Continuously evaluate your program and focus campaigns, strategies, and challenges on the most impactful area. Another sure-fire way to keep participation high is to include program elements the participants actually want. Provide surveys, focus groups, and wellness committee communication. Giving your users the opportunity to have a say and provide feedback helps them take ownership and feel it is THEIR program. This also applies to incentives. Prizes are great, but only if they are things people actually want!
Get started on your company’s wellness program by scheduling a free demo with our team today!