Executive Summary
What is the best wellness program for employees?
The best wellness program is one that improves employee health while delivering measurable results for the organization—with expert guidance built in. Programs supported by experienced wellness professionals are more effective because they provide structure, accountability, and data-driven adjustments over time. With expert guidance, wellness efforts lead to higher participation, healthier behaviors, stronger morale, and meaningful reductions in healthcare costs.
What does it take to build one of the highest-rated workplace wellness programs in the U.S.?
The C. Everett Koop Health Project identifies the nation’s best wellness program each year. Specifically, the Koop Award recognizes the top wellness programs. For instance, the Koop Award, for the nation’s top wellness program, honored Boise School District and their partner WellSteps as the nation’s top wellness program.
So here is the blueprint that shows exactly what it takes to have the one of the highest-rated wellness programs in the U.S.
Where should organizations start when building a high-performing wellness program?
In 2011 Boise School District had over 3,000 employees dispersed over 58 geographical locations. District employees had been experiencing an increased prevalence of poor health behaviors, elevated health risks, and consistently increasing health care costs.
As a response, that year the district made the strategic decision to implement a comprehensive worksite wellness program. Moreover to achieve this, and to help plan, implement, administer and evaluate the wellness program, the district contracted with WellSteps.

Undoubtedly, the Boise School District designed its wellness program to help employees improve health behaviors. And, to make the overall work culture more supportive of good health practices. Thus, the program provided employees with the awareness, education, motivation, tools, strategies, supportive policies and social support needed to adopt and maintain healthy behaviors.
The program incorporated administrative planning, baseline data evaluation, culture change and communication strategies, biometric screening, behavior change campaigns, and incentive tracking. For example, district offered four behavior change campaigns lasting four to eight weeks each year.
Certainly, these campaigns aim to improve health behaviors and build self-efficacy by breaking the the behavior change process to manageable weekly tasks. The district, specifically, designed the program to maximize employee engagement and impact.
Researchers have subjected few employee wellness programs of this size to such a high level of scrutiny. Yet, to date, the district has published four four different program outcome evaluations.
This application reviews the program design as well as the one, two, and three-year outcomes associated with changes in employee health behaviors, elevated health risks, health care costs, and self-reported measures of job performance and job satisfaction.
In short, the program has produced evidence. Evidence of improved nutrition, physical activity, sleep quality, and reductions in tobacco and alcohol usage. Moreover, it has demonstrated reductions in stress and depression, and improvements in life satisfaction.
The program also appears to have reduced elevated levels of systolic and diastolic blood pressure, cholesterol, and glucose. Furthermore, evaluation of six years of medical claims data showed that wellness program participants cost significantly less than non-participants.
In reality, for every dollar the district spent on wellness programming, it saved $3.50 in health care costs. From 2009 to 2014, the district’s health care cost remained stable. Finally, The district demonstrated that healthy behaviors significantly reduced presenteeism and increased job performance and job satisfaction.

As a publicly funded entity, Boise School District has demonstrated that its investment in employee health and wellness has significantly improved employee health and reduced employee health care expenses.
The district’s wellness program has surely been a benefit to district employees, their families, and the tax paying citizens of Boise, Idaho.
What can employers learn from the Boise School District wellness program?
Starting in 2011, Boise School District began offering a comprehensive employee wellness program to its 3,284 eligible employees. As a result, the district has enjoyed many successes and positive outcomes with its wellness program. Furthermore, they hope to share their formula for success with other similar organizations.
Boise School District ranks second in its state in size. Specifically, the district includes six high schools, eight junior high schools, and 31 elementary schools. Notably, each employee is located in one of the 58 locations within the district.
Above all, the aim of this multi-year program was to improve employee health behaviors, lower elevated health risks, prevent chronic diseases, and curb rising healthcare costs. To achieve this, the district developed a comprehensive and strategic approach.
The district program was certainly unusual in that it applied to multiple locations and the majority of the employees were teachers. In reality, little evidence was available that demonstrates the impact of a well-designed wellness program on this specific population segment.
In 2011, approximately 73.3% of employees were female and the average age was 48.6 years. From 2011 to 2016, the district left the benefits design plan unchanged except for the addition of incentives for wellness program participation.
Employees and spouses could qualify for lower premiums, co-pays, and deductibles when they participated in the program. In essence, baseline health risk appraisal data revealed that this employee population mirrored the health risks and behaviors of other employee populations located in Idaho.
The district also made the program available to spouses and retirees (employees who retired from the district but were not yet eligible for Medicare). The program began in the fall of 2011.
What distinguishes a nationally recognized wellness program?
Boise School District hired WellSteps LLC to provide the design, implementation, administration, and evaluation of its wellness program. The decision to hire a vendor was based on limitations within the district due to its size, budget, and lack of wellness support staff.
The decision was also based on the fact that the district’s insurance carrier provided access to a variety of population health management tools such as case management, a nurse hotline, an EAP, and disease management, but not wellness.

This wellness model combines elements of the RE-AIM Framework and the AMSO Model proposed by O’Donnell. In sum, the model includes the essential elements of an effective wellness intervention in an easy-to-explain and understand format.
In truth, researchers may have developed more scientifically grounded intervention models. But, they are not as simple to explain or apply in a worksite setting.
This model’s driving philosophy asserts that employee-related expenses such as absenteeism, presenteeism, and medical costs are heavily influenced by poor employee health.
Elevated health risks, primarily driven by poor lifestyle choices, directly cause poor health. Therefore, to impact employee-related expenses, wellness programming must focus on the root cause of poor health ─ unhealthy behaviors.
To do this, the program relies on two foundational elements of a successful wellness program: Reach and Impact. Now, reach is the ability of the wellness intervention to reach every single eligible employee. And then reach them with the correct messaging, the correct communication channel, and the correct call to action. All executed at just the right moment.
The most effective worksite wellness interventions are of no value if they do not reach employees. Program design and ease-of-use dramatically impact reach.
To maximize reach, the district streams every component of the wellness program to mobile devices or computers. Additionally, the programming is available in multiple languages.
Many employees and significant others complete the personal health assessment and behavior change campaigns using a mobile device. Focus groups test each intervention and user interface to ensure the program meets its goal of ease-of-use.
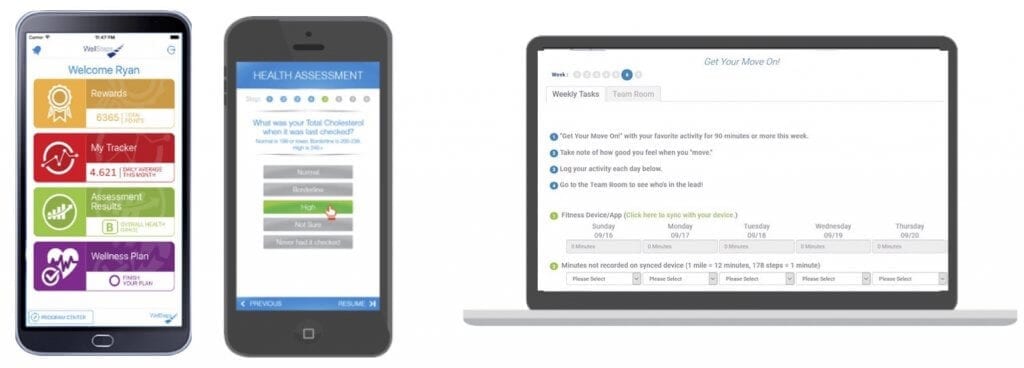
Experts technically define impact as the effect size of the intervention. The wellness program impacts employees because it provides all the education, awareness, motivation, tools, strategies, supportive policies, and social support needed to help employees adopt and maintain healthy behaviors.
With effective reach and impact, the wellness program is able to improve health behaviors, reduce elevated health risks, lower chronic disease prevalence, and impact employee-related expenses. Program designers create every component to focus on and maximize both reach and impact, helping organizations maximize the effectiveness of their wellness programs.
A key element of the program is the use of technology to facilitate program delivery and administration.
Rather than rely on a stand-alone wellness web portal, the wellness program is an interactive behavior change platform. The platform uses social media, video, weekly tasks, quizzes, team competitions, wearable device integration, goal-setting, reminders, text messaging, push notifications, and incentive tracking to promote healthy behaviors.
This leveraged technology platform provides a careful blend of user convenience and face-to-face interactions with other program participants. For example, in the Move It Coast to Coast campaign, participants work together as a team. They support each other engaging in physical activity as their team competes with others to “race” across the United States.
This campaign uses behavior change strategies and social support to help all team members increase physical activity. Furthermore, it applies technology to track progress and enable communication within and between teams.
The technology enables the wellness program to provide the same interventions to employees working at 58 locations. It ensures a high level of wellness program fidelity across a geographically dispersed workforce.
Why are leadership and culture change essential to building the best wellness program?
The district has demonstrated considerable leadership support for wellness. The district superintendent, benefits directors, benefits committees, and managers had previously decided to make creating a healthy workplace a district priority. The organization created budgets and allotted time for all employees to learn about and participate in the wellness program.
Each year, mandatory meetings included substantial discussion and introduction to wellness programming and healthy living. District leadership also designated a district wellness committee and charged the committee with assisting in the design and implementation of the wellness program.
Planning the various aspects of the district wellness program involved collection and evaluation of district health insurance claims data, input from the wellness committee and district wellness coordinator, and aggregate HRA data received from a previous insurance carrier. Planners used all of this to design and administer the wellness strategy.

How should wellness programs be communicated and implemented effectively?
The school district wellness program began with extensive program pre-implementation. The organization initiated a marketing campaign four months before launching the program. This campaign included visible leadership support for the wellness program, posters, postcards, emails, newsletter articles, blogs, and department announcements.
The organization mailed postcards announcing the program to each employee’s home to notify spouses and significant others. Leaders introduced and explained the wellness program to all employees during the required fall meetings.
Table 1 shows each of the implementation components. To begin with, the program incorporated administrative planning, baseline data evaluation, culture change and communication strategy, biometric screening, behavior change campaigns, and more. In addition, program organizers offered four different behavior change campaigns, each lasting four to eight weeks, every year.
Specifically, campaign designers aim to improve health behaviors and build self-efficacy by breaking the behavior change process into manageable weekly tasks. For instance, these campaigns may include short videos, simple quizzes, games, materials, wearable device integration, demonstrations, team competitions, behavior change strategies, incentives, and peer support. As shown in Table 1, a sampling of the program components highlights the comprehensive approach to the initiative.
TABLE 1. WellSteps Wellness Program Components
| Intervention | Description |
|---|---|
| Personal Health Assessment (PHA) | Before participating in the program, employees completed a self-reported Personal Health Assessment (PHA), after which they received individualized electronic feedback. Aggregate data is used in program design and evaluation and is collected every year. |
| Culture Change Strategies | To create a healthy culture, the district used the Checklist to Change. This free culture audit tool helps worksites assess health-promoting policies and environments. Each quarter, the onsite wellness program coordinator and wellness committee use these results to identify one policy or environmental support to implement. Each year, the district made multiple environmental changes including vending machine changes, cafeteria changes, creation of walking paths, and rules for healthy birthday food celebrations. |
| Rewards | Rewards is an incentive management platform. Employees earn points and progress towards the benefit-based incentive when they complete program requirements such as the PHA, biometric screening, or campaign completion. Rewards automatically tracks, reports, and updates each employee’s incentive progress. Employees can also use the app or program center to report completed items or verify completion by submitting documentation. Rewards helps each employee see their incentives progress. |
| My Tracker | Regardless of the wearable device an employee may have, My Tracker automatically syncs all wearable devices and displays activity data in each employee’s dashboard. My Tracker also automatically uploads wearable data to the Rewards incentive platform. District employees who have wearable devices can automatically get credit for being active. |
| Biometric screening | Each year, the district requested that each employee complete a biometric screening. This could be done onsite or by any employee’s primary care provider. To submit proof that the screening was completed, employees could fax, email, or use the app to image and upload the screening form. |
| Disease Management | Employees who indicated that they had diabetes, cardiovascular disease, or asthma could participate in specific disease management challenges. The challenges are two-week behavior change programs designed to help employees adhere to care recommendations, medication management, and work towards adopting and maintain healthy behaviors. |
| Screening Reminder | Using age and gender data from the PHA, each employee received emails and text messages reminding them to get their age and gender specific cancer screenings. Many district employees received incentive points when they completed the appropriate screenings. |
| Behavior Change Campaigns | |
| The Culprit and the Cure | Participants apply science-based healthy lifestyle principles from The Culprit and the Cure. Weekly tasks include reading and quizzes, watching brief video vignettes, reviewing personal assessment results, setting change goals, teaching friends or family key principles, and sharing the book with someone else at the end of the campaign. |
| Fast Food Nutrition Guide | Participants learn to use the Fast Food Guide to make healthy fast food choices. Weekly tasks include reading and quizzes, going out to eat with others and using the guide to make a healthy choice, practice rating foods, and sharing the book with someone else at the end of the campaign. |
| Move It! Coast to Coast | Participants compete with coworkers to engage in 30 minutes of physical activity at least 3 days a week for 6 weeks. Weekly tasks include watching a video about the benefits of exercise, logging steps or minutes, team meetings, and team exercise, when appropriate. | Boosting Mental Health | Participants will learn the basics of mental health, as well as how to manage stress, improve sleep, proper nutrition, and adequate exercise. They will learn how these changes can improve mental health and set goals to integrate them into their own lives. |
| Good Night | Participants make changes in their sleep habits, routine, and environment to improve sleep quality. Weekly tasks include watching brief video vignettes, assessing pre-sleep behaviors, setting sleep goals and schedules, modifying sleep environment, and journaling. |
| Maintain, Don’t Gain | Participants apply strategies to manage caloric intake and to increase energy expenditure during the holidays. Weekly tasks include weighing in and applying behavioral strategy to manage weight. |
| Food Makeover | Participants modify their home environment by replacing unhealthy food with healthier options. Weekly tasks include watching brief video vignettes, assessing and changing food environment at home, applying healthy substitutions at the store, making and using a shopping list, and finding and preparing healthy recipes. |
| Stress Free | Participants learn to identify and manage stressors by applying simple strategies. Weekly tasks include watching brief video vignettes, assessing common stressors, practicing a stress management technique, applying strategies to eliminate or reduce stressors. |
| Posture Perfect | Participants learn how to avoid injury with proper lifting techniques and posture. They inventory the workspace for stressors and learned how to properly sit and stand. |
| Sugar Busters | Participants watch a few short videos that will help them recognize the many forms of sugar. They learn how to avoid hidden sugar and are invited to replace sugary breakfasts and desserts with healthier options, to apply “sugar busting” substitutions, to prepare a healthy recipe, and to hide or throw out a high-sugar food. |
| Overcome Overeating | Participants watch several brief videos about strategies that people use to overcome overeating. They are taught to identify the foods, cues, and situations that influence eating and complete weekly tasks to apply what they learned. |
| Good Fat Bad Fat | Participants are taught about types and sources of unhealthy fats and healthy fats. They also prepare healthy meals that include the use of good fats. |
| Balance It All | Participants watch a short video about priorities then take the “the Big Rock” assessment. They learn how to plan around priorities, how to say “No,” how to schedule time for themselves, and how to delegate. |
| Incentives | |
| Campaign Specific Incentives | Five percent of the wellness budget is dedicated to incentives. Gift cards, event tickets, prizes, and gifts are awarded to a random selection of employees who complete a campaign. These incentives are immediate, small, and external incentives. In addition, all campaign participants are encouraged to understand, recognize, and enjoy all of the intrinsic benefits that accompany healthy behaviors. The goal of these small incentives is to help employees stay motivated as they start to identify and enjoy the intrinsic benefits of a healthy lifestyle. |
| Benefits-based Incentives | In 2011 and 2012, employees who completed the PHA and biometric screening qualified for a $20 lower office copay, a deductible that was reduced from $700 to $350, and a $40/month premium discount. In 2013, employees were asked to also complete at least one behavior change campaign or approved alternate activity. As with the small incentives, each employee was shown how to identify and appreciate all of the intrinsic incentives that come from healthy living. |
Evaluation Methodology and Results for the Koop Award
The Boise School District wellness model is based on the notion that poor health behaviors lead to elevated health risks. Elevated health risks are the primary driving factors behind high chronic disease prevalence. They also elevate employee-related expenses such as medical costs, prescription costs, and productivity losses.
Thus, improving unhealthy behaviors should be the focus of every program. This same model can also be applied to the evaluation of the program.
Because program evaluation has been built into the very foundation of the model, there are many opportunities for program evaluation. To date, data from the district’s wellness program have resulted in four independent, peer-reviewed publications.
Program evaluation first involved looking at descriptive data on program participation and engagement. Next, the impact of the program on unhealthy behaviors and elevated health risks was determined.
Finally, the program was evaluated to determine the impact on health care costs, productivity, and job satisfaction. Brigham Young University researchers completed the evaluations. Each evaluation has published or been accepted for publication in the health promotion scientific literature.

What results should employers expect from a well-designed wellness program?
Several methods and approaches were utilized to measure program participation. Employees who were able to complete the personal health assessment, biometric screening, and complete at least one behavior change campaign each year qualified for the district’s wellness incentive.
This incentive included a $20 lower office copay, a $40 lower monthly insurance premium, and a lower insurance deductible ($350 vs $700 per year).
In 2011, 2012, and 2013, participation increased from 65.6% to 74.1% to 81.1%, respectively. In 2013, there were 3,282 eligible employees. Of those, 80% completed the personal health assessment, 81% completed a biometric screening, and 59% completed at least one behavior change campaign. Most employees completed 2 or more campaigns.
How do effective wellness programs improve health behaviors?
The Personal Health Assessment (PHA) includes 30 health and lifestyle questions that are modified from the Behavior Risk Factor Surveillance System. The PHA can be completed online, using the mobile app, or via paper and pencil. Furthermore, the evaluation of health behaviors required three successive PHA completions: baseline, and year 1, and 2.
Table 2 shows changes in health risks across all three time periods. This analysis includes all employees who completed the PHA three years in a row. One and two year improvements were seen in exercise, fruit and vegetable consumption, days of quality sleep, tobacco and alcohol use, and self-rated health.
As illustrated in Table 2, changes in health risks were tracked across all three periods of time. Notably, this analysis shows significant improvements in mental health-related outcomes such as stress, depression, and life satisfaction. This two year evaluation is currently in press with the journal Preventive Medicine.
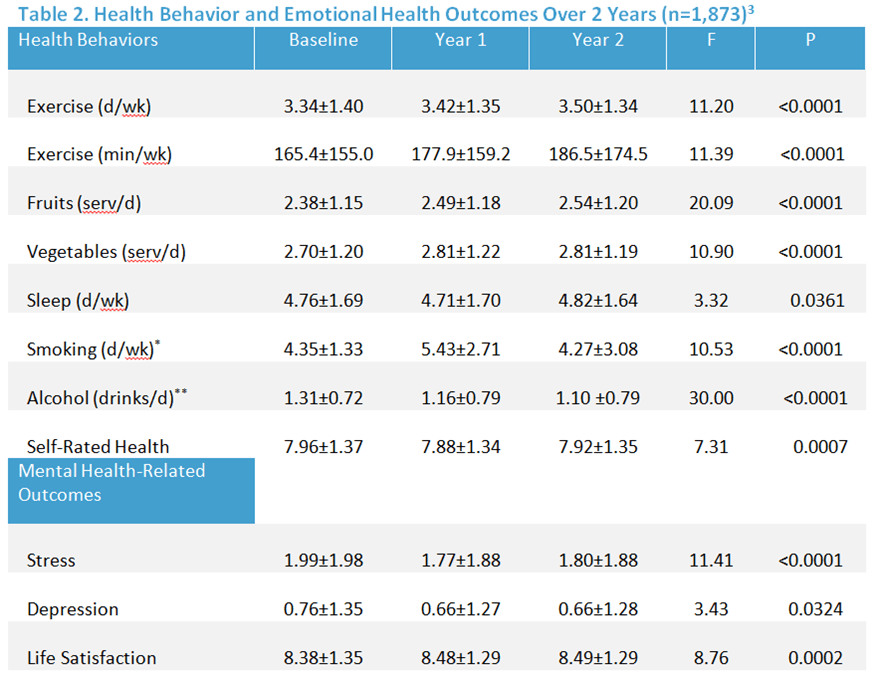
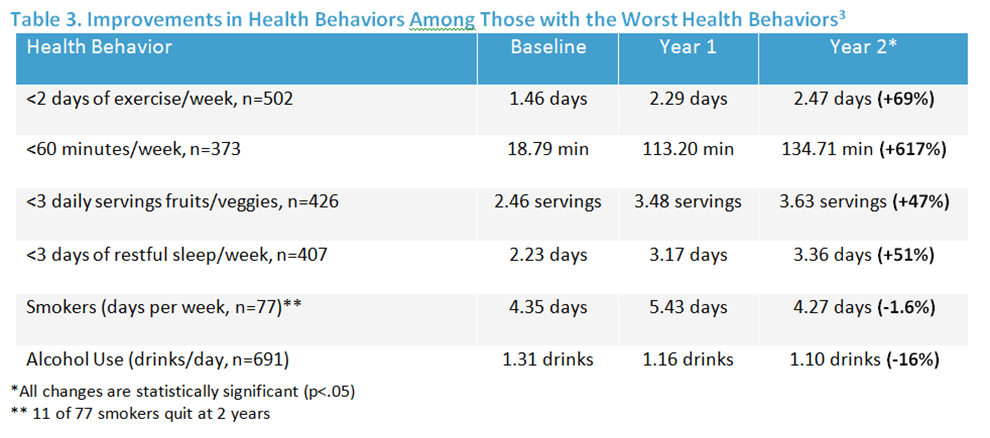
Table 3 shows, clearly, the program impact on individuals who had the worst health behaviors at baseline.
After 12 and 24 months, dramatic improvements were seen. Specifically in those employees who had previously reported low levels of baseline exercise, fruit and vegetable consumption, days of restful sleep, and high levels of tobacco and alcohol use.
How do wellness programs reduce elevated health risks?
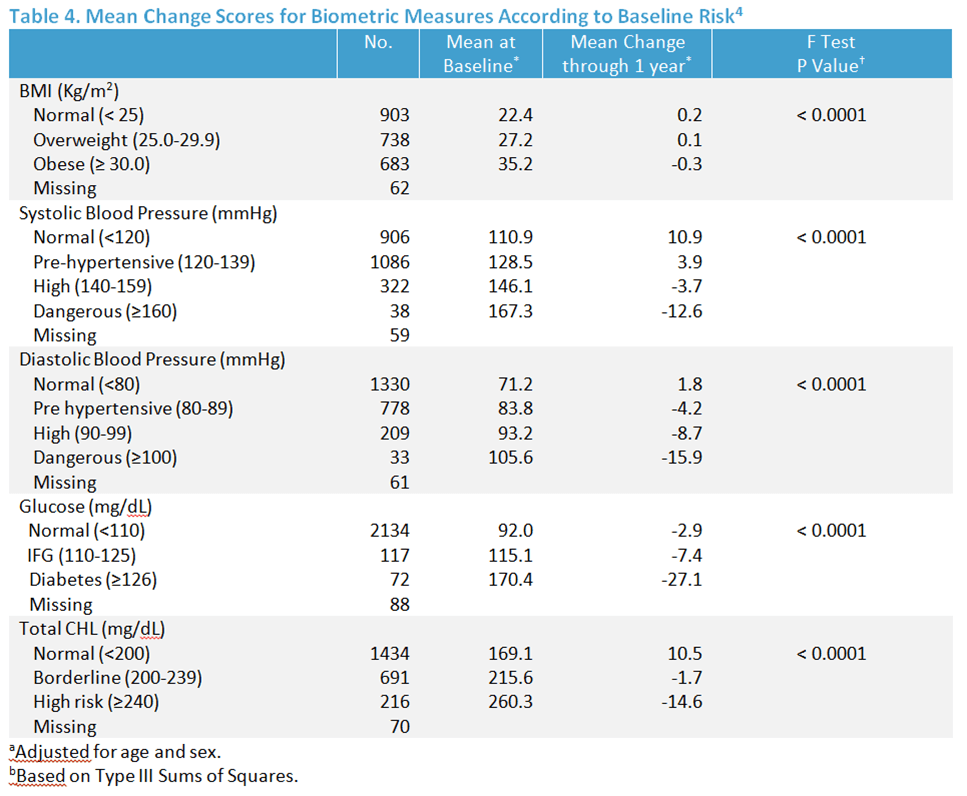
Evaluation of health risk changes was based on repeated measures data from 2,411 employees.4 Participants’ BMI, SBP, DBP, glucose, and total cholesterol levels were measured at baseline and again after one year.
Specifically, the numbers of high risk employees at baseline were 683 for BMI, 360 for SBP, 242 for DBP, 72 for glucose, and 216 for total cholesterol. Among participants, 47.4% lowered BMI, 36.2% lowered systolic blood pressure, 57.4% lowered diastolic blood pressure, 66.9% lowered blood glucose, and 40.4% lowered total cholesterol.
The percentages moving out of the high risk categories after one year were 11.4%, 39.4%, 70.7%, 38.9%, and 40.7%, respectively. Table 4 shows changes in biometric health risks. Importantly, there was consistent risk reduction among those who had the unhealthiest numbers at baseline.
How do wellness programs impact healthcare costs over time?
Health care cost data for school district employees during the academic years 2009 through 2014 were linked with wellness program participation status. But, additional program information was obtained from health risk appraisals and biometric screenings conducted in the academic years ending in 2012 through 2014.
The main outcome measures were claim frequency and cost of medical claims. The Preventive Medicine Reports, Volume 3, June 2016, published the complete evaluation.
Individual wellness program participation data were then combined with individual medical cost data. This allowed for comparison of the medical costs between wellness program participants and non-participants.
Six years of medical cost data were evaluated, including the three years prior to wellness program implementation.
The “pre-program” cost data was used to statistically remove pre-existing differences in cost between participants and non-participants. During the three-years prior, program non-participants had slightly higher medical costs ($3,414 vs $3,308).
No differences existed in age or sex between participants and non-participants. Post-implementation, there was a dramatic difference in the cost of medical care between wellness program participants and non-participants. This is specifically seen in 2012 and 2013 and to a lesser extent in 2014. (Table 5)
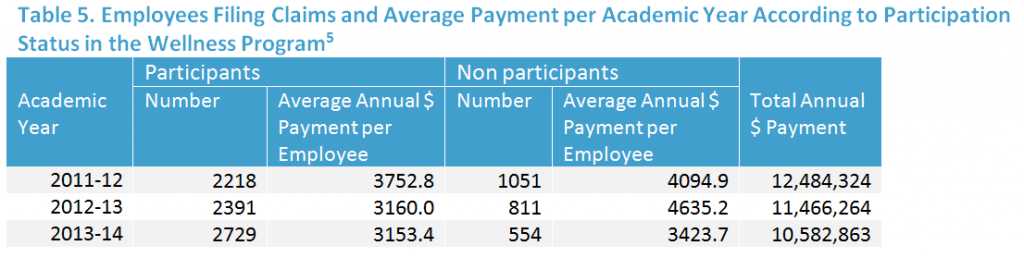
From 2012 to 2014, the program participants cost the district $5,025,138 less in medical costs than non-participants. It is highly likely that this cost savings is primarily due to the impact of the comprehensive wellness program.
The cost of providing the wellness program during the same three year period was $1,412,736. After subtracting program costs, the cost savings from the wellness program was $3,612,402. Thus, the benefit to cost ratio for the program was 3.56 ($5,025,138/$1,412,736). During this study there were no changes in the district’s health plan design.
As shown in Figure 1, the predicted medical costs had the district followed the same cost trends of comparable worksites. In short, this prediction provides a good estimate of what the cost trend would have been in the absence of a wellness program.
But the district did not experience the predicted trend of comparable worksites. Rather, district medical costs peaked in 2011, and then decreased each year through the end of the evaluation period (2014).
The district medical costs in 2014 ($11,390,481) were lower than the costs in 2009 ($11,590,407) demonstrating a zero trend across the six-year evaluation period.
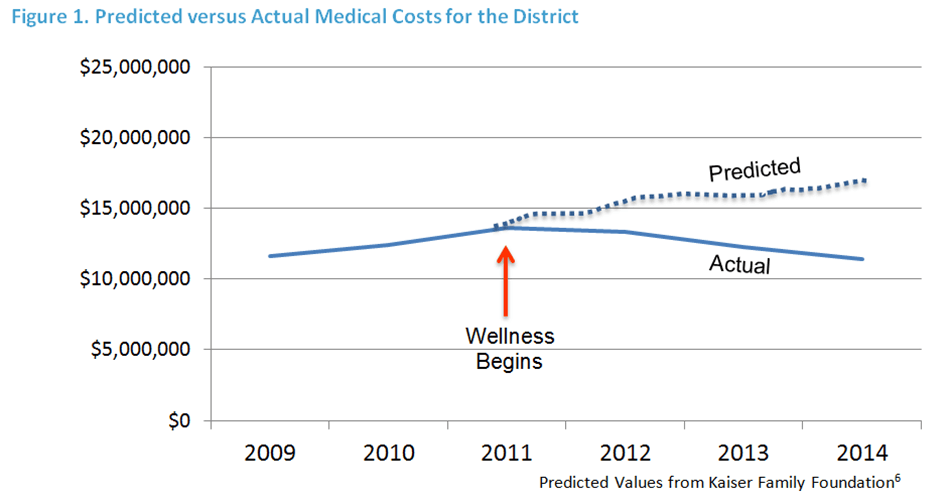
Figure 1. Predicted versus Actual Medical Costs for the District
How do wellness programs influence productivity and job satisfaction?
To further evaluate the relationships between employee health behaviors and employee job performance, absenteeism, and job satisfaction, an additional evaluation was performed. This study examined the association between selected health behaviors and work-related outcomes among 2,395 district employees.
Those who exercised at least five days per week, exercised 150 or more minutes per week, consumed five or more fruits and vegetables per day, or obtained five or more restful days of sleep per week, exhibited higher job performance, life satisfaction, self-rated health, and job satisfaction and lower levels of absenteeism, depression, stress, and loneliness (P<0.05) than those who did not.
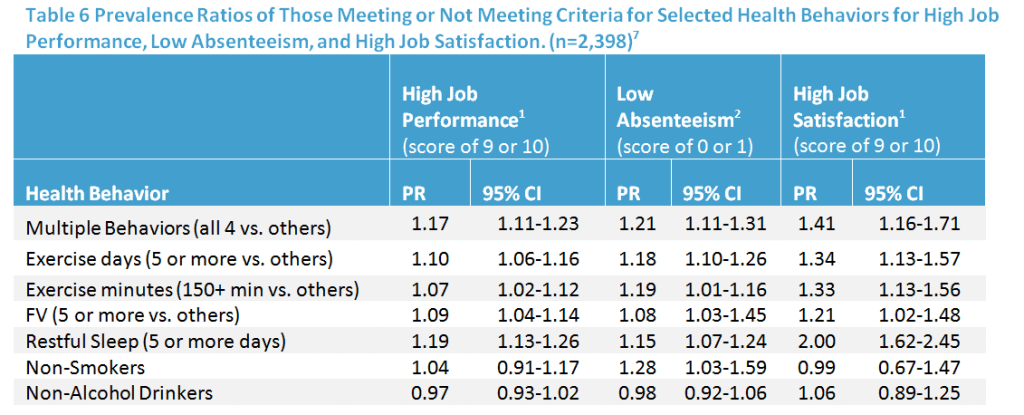
Employees who reported achieving defined levels for the above four health behaviors simultaneously reported higher job performance (Prevalence Ratio=1.17; 95% CI=1.11-1.23), lower absenteeism (Prevalence Ratio =1.21; 95% CI=1.11-1.31), and higher job satisfaction (Prevalence Ratio =1.41; 95% CI=1.16-1.71).
These results indicate that selected healthy behaviors, individually and when co-occurring, are significantly associated with productivity, satisfaction, and emotional health outcomes. Table 6 shows the prevalence ratios between each health behavior and each work outcome.
Furthermore, these data provide additional evidence for the need to keep the wellness program focused on helping employees adopt and maintain healthy behaviors. In sum, they also help support the business case for a comprehensive wellness effort.
What conclusions can employers draw from top-performing wellness programs?
The WellSteps wellness program is an evidence-based program, carefully adhering to the RE-AIM and AMSO behavior change frameworks. With the completion of several published evaluations, the program is also evidence producing.
Certainly, these published evaluations demonstrate that the program helped district employees adopt and maintain healthy behaviors and reduce elevated health risks.
The program also had a meaningful impact on the district’s medical cost trends. Boise School District has been able to demonstrate that a well-designed, comprehensive wellness program can be an effective and cost-effective way to improve employee health and reduce employee medical expenses.
When taken collectively, this research proves that Boise School District and WellSteps are worthy of the Koop Award. Even more, the label as the one of the nation’s best wellness programs. So, why not schedule a free demo with our team today to get started?
Frequently Asked Questions
The best wellness program combines simplicity, personalization, strong communication, and leadership support. Employees feel guided rather than pressured, and the program builds habits gradually instead of feeling forced to change.
Companies can improve an existing wellness program by adding fresh activities, updating incentives to keep them meaningful, and increasing opportunities for employees to personalize their experience. Regularly checking in on what people actually need makes a big difference, and tools like the WellSteps Personal Health Assessment help identify priorities so the program can evolve with the workforce.
Top wellness programs stand out because they are consistent, transparent, and engaging. They provide clear, meaningful rewards that motivate participation, offer a variety of activities to keep employees interested, and adapt to changing needs over time. These programs also foster a culture of well-being by integrating wellness into daily work life, encouraging participation at all levels, and using data to continuously improve results.
The easiest approach is using an all-in-one platform like WellSteps that includes tracking, challenges, incentives, and reporting. This replicates the structure used by organizations with award-winning programs.

