Executive Summary
How do hospital wellness programs support staff health and patient care?
Hospital wellness programs support staff health by reducing burnout, improving morale, and helping employees manage physical and mental stress in high-demand environments. These programs work best when they are easy to access, flexible across shifts, and supported by leadership. Over time, healthier staff leads to better retention, fewer absences, and more consistent patient care. Investing in employee wellness helps hospitals care for caregivers so they can better care for patients.
Why should hospitals offer wellness programs to employees?
Hospitals, clinics, and other health care providers are just like any other businesses – they need to manage large numbers of employees and control expenses, while delivering needed services. While some health care providers are struggling to stay competitive, the most successful ones offer health and wellness programs to their employees.
Most healthcare professionals, though, take great pride in their work. And, they often put patients first and make their job a priority over other things, including their personal health. This is admirable, but comes with a price.
Hospital settings are excellent places to offer wellness programs for healthcare workers because they struggle with their own health. This does not have to happen. Just because a person chooses to work as a healthcare provider doesn’t mean that their personal health should suffer.

Do healthcare workers experience higher obesity rates than other occupations?
Every day healthcare workers watch patients experience the pain and suffering that results from poor lifestyle behaviors and unhealthy living. Hospital wellness programs should be implemented in every healthcare setting because healthcare workers have some of the nation’s highest health risks.
Healthcare workers are acutely aware of what happens to those who use tobacco, don’t exercise, or suffer with obesity. And yet, healthcare professionals have some of the highest rates of elevated health risks compared to the rest of the population.
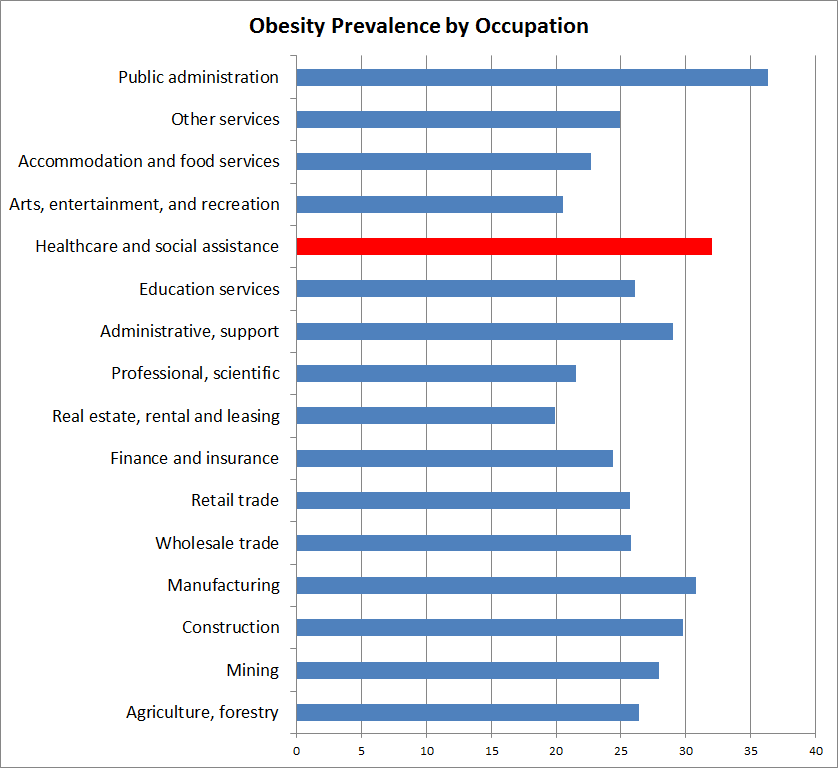
In summary, the table below demonstrates the prevalence of obesity among different professions. With the exception of those who work in public administration, healthcare professionals have some of the highest rates of obesity.
Over 32% of those who work in healthcare have a higher than recommended weight. This rate of obesity is higher than just about any other occupation. This data includes only those who have a body mass index greater than 30.
A study of hospital workers in Texas showed that 78.1% of healthcare workers have a body mass index [BMI] ≥25.0 kg/m2) Stated another way, 4 out of every 5 healthcare workers in the state of Texas have a higher than recommended weight. These employees had high rates of hypertension, high blood glucose, and high blood cholesterol.
It’s pretty clear from the research that those who work in the health care industry have dramatically higher rates of obesity. Why is this so?
Why Do Health Care Professionals Struggle with Excessive Weight?
When compared to those who are normal weight, healthcare employees with higher than recommended weight eat more starchy foods, fats, and sugary beverages. They spend more time watching television, playing computer games, and sitting than their normal-weight counterparts.
Studies that have focused specifically on nurses have shown that those who are struggling with weight are more likely to be involved in shift work and long work hours. They report having to work in a high-stress environment where there is psychological, emotional, and physical demands.
Not surprisingly those who are suffering from weight are also more likely to report work-related musculoskeletal injuries and pain. It’s hard to tell which comes first: the work-related injuries or the excessive body weight.
It’s clear that healthcare workers have a significantly higher rate of obesity compared to other workers, and high rates of obesity in this group is just the tip of the poor health iceberg.
Evidence also suggests that healthcare workers also have very poor diets and fail to get adequate physical activity. It appears that the excessive weight is most likely caused by a combination of factors including high amounts of stress, poor nutrition, and lack of regular physical activity—all behaviors that are directly impacted by wellness in healthcare.
Do healthcare workers face higher rates of chronic disease?
The connections between lifestyle behaviors, elevated health risks, and chronic disease are all well documented. In short, employees with elevated health risks are more likely to develop chronic diseases.
That is exactly what the research findings show. Health care workers and their dependents are significantly more likely to be diagnosed with depression (20% higher) and asthma (12% higher), including higher admission rates for the treatment of asthma.
Looking at over 350,000 healthcare workers, researchers were able to demonstrate significant differences in chronic diseases. Healthcare workers are, in sum, much more likely to have and struggle with chronic diseases. This fact alone can explain much of the difference in health care costs that are experienced by healthcare workers.
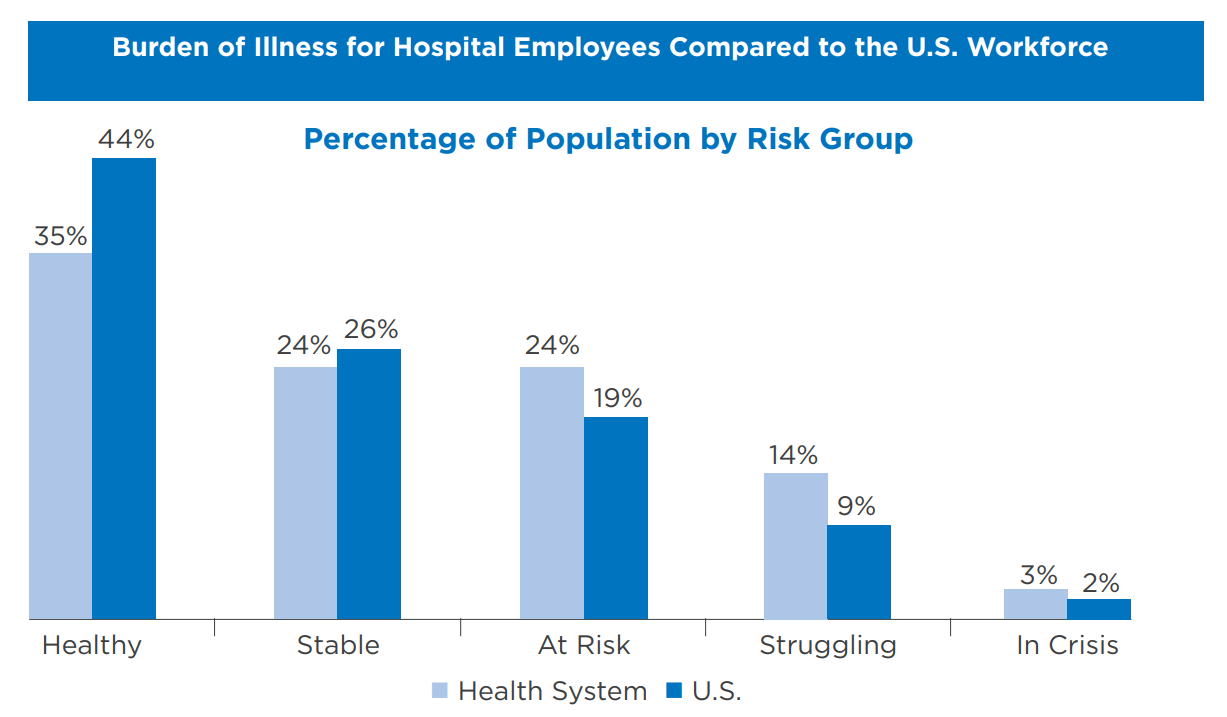
3. Health Care Workers Have Dramatically Higher Health Care Costs
However, as might be expected, healthcare workers who have elevated health risks, like obesity, are more likely to have chronic diseases and subsequent healthcare costs. And, this is exactly what the research demonstrates. Several large studies looked at the healthcare costs of 1.1 million healthcare workers and compared these to the healthcare costs of 17.8 workers from other occupations.
Medical care and prescription drugs costs for healthcare workers are 10% higher than the general employee population and 13% higher when employees’ dependents were included.
This dramatic difference in the cost of healthcare is even more troubling when you consider the average age of the typical healthcare professional. Health care workers tend to be younger females with an average age of almost 2 years younger than the average US worker. Despite the fact that younger employees use less healthcare, the cost of medical care for healthcare workers is significantly higher than the cost for other employees.
Hospital wellness programs for employees that focus on reducing elevated health risks have been shown to have a direct impact on the cost of healthcare. This is one of the most important reasons why wellness in healthcare is so important.
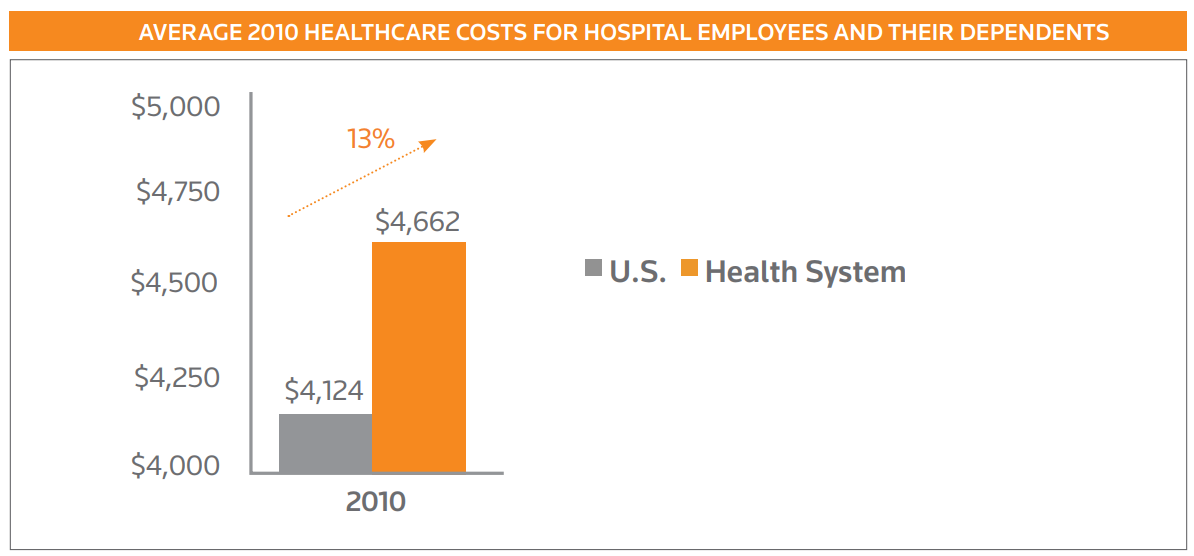
Lowering health risks is exactly what successful hospital wellness programs do. In fact, hospitals that use WellSteps wellness solutions get a performance guarantee that health risks will be reduced by 7% after just two years.
How do stressful work environments affect healthcare workers’ health?
Genetically, healthcare workers are pretty much like everybody else. They may be slightly younger, more educated, and may have more females in the population but this alone cannot explain why they are less healthy.
The main explanation for the high rates of obesity in health care costs has to do with the cultural and environmental factors they face at their places of work. For example, depending on the specific job some healthcare professionals may be sedentary or they may do a lot of on-the-job walking.
One study found that hospital nurses walked 4–5 miles during a 12-hour shift and 1/3–1/2 mile per hour worked. In many cases this includes a lot of stair climbing. On the other extreme, some healthcare workers are completely sedentary during their entire shift.

Nutrition plays perhaps the biggest impact on poor health. Historically, healthcare workers would typically bring their own lunches, which could include sandwiches and some fruit. Today, very few healthcare workers bring their own lunches, preferring to consume foods found in vending machines or in the cafeteria.
To make matters worse, the families of patients often bring in treats or candy. These gestures of appreciation are well intended, but the consequences may be unwanted. A survey of hospital nurses found that the nurses were consuming an average of 5.4 chocolates each day. When asked why they consumed so much, the most common response was the simple fact that “they were there.”
Another reason for the poor nutrition of healthcare workers is the lack of time available to have a healthy lunch. Rather than sit down at a planned nutritious meal, many workers might just grab a snack or fast food item from a vending machine.
Many healthcare workers complain about the amount of stress that they experience in the worksite. It is often believed that high amounts of psychological stress could lead to poor work performance and elevated health risks. It is still unclear whether high amounts of work stress contribute to high rates of obesity.
Once again, a well-developed hospital employee wellness program can have a direct impact on employee physical activity, nutrition, and stress. These three risk factors should be the core of most hospital wellness programs.
Do healthcare workers use emergency and hospital services more frequently?
A trip to the emergency room costs an average of $1,233. That’s about 40 percent more than the average American pays for rent ($871 per month). This is a problem for healthcare workers because they and their dependents are 22% more likely to visit the emergency room than other workers.
Healthcare workers are hospitalized 5% more than the US average, and they stay in the hospital for 18% more time.
During these emergency room and hospital admissions they are more likely to be treated for chronic diseases such as depression, asthma, diabetes, obesity, coronary artery disease, congestive heart failure, hypertension, and back and spine disorders.
The reason healthcare workers are more likely to use health care is because they are more familiar with how healthcare works. However, many healthcare providers will seek healthcare services for the procedures and conditions they are familiar with. It’s as if familiarity with the business of healthcare increases the odds that they will use that healthcare.
Though, in my opinion this is the single biggest reason why healthcare workers have dramatically higher health care costs. They are familiar with the processes and procedures used in the medical community and they don’t hesitate to use them.
The best wellness programs are effective at improving employee health and reducing the incidence of chronic diseases. So this means program participants have lower use of medications and hospital visits. This translates into lower health care expenses for both the employees and the employers.

Why are hospitals extending wellness programs to the community?
Not only are hospitals and healthcare settings likely to offer health care wellness programs for their employees, but they are increasingly more likely to offer the same services to people and their communities. The number of hospitals offering health and wellness programs to people in the community increased from 19% in 2010 to 66% in 2015.
WellSteps works directly with many of these healthcare providers. In fact, they use the WellSteps wellness solutions to improve their health of their own employees and they market these same services to businesses and worksites in their community.
They do this for two reasons:
1) Firstly, hospitals are offering wellness services in the community as part of their marketing and branding strategies. People see hospitals promoting wellness, and they associate high quality of life and good health with those who use those hospitals.
2) Secondly, hospitals are using wellness programs as a revenue generator. They’re doing wellness to make money. Along the way they can build partnerships with worksites and communities; not only are they good at treating disease, they’re making efforts to prevent disease from ever happening.

In summary, to offer an effective hospital wellness program hospitals need to provide 3 things:
- Staff that is qualified to plan and administer the program
- Effective behavior change interventions and activities
- A web-based data platform on which to administer, communicate, and evaluate the program.
However, few companies do all three. But, that’s why the fastest growing segment of the wellness market is the reseller market. Health care provides who want to do wellness for their own employees or for employees in the community will use a wellness software platform. They deliver the wellness program with the right technology without having to develop the technology.
Here is how many hospitals have become wellness resellers.
What evidence shows hospital wellness programs are effective?
In 2015, about 87% of hospitals reported that they were doing at least some health and wellness program or other initiatives for employees. Few of these programs are comprehensive, but at least they are a start. A comprehensive hospital wellness program offers a complete wellness solution.
Among hospitals that offer a full wellness program, here is a list of activities they do and how many hospitals offer them.
What some of the best hospital wellbeing programs are doing:
| Health risk assessment | 82% |
| Biometric screenings | 72% |
| Safety program | 92% |
| Flu shots or other immunizations | 100% |
| Stress management | 74% |
| Disease prevention/management programs | 77% |
| Healthy food options | 93% |
| Weight loss programs | 77% |
| Gym membership discounts | 79% |
| On-site exercise facilities | 64% |
| Smoking cessation program | 85% |
| Personal health coaching | 62% |
| Classes in nutrition or healthy living | 72% |
| Web-based resources for healthy living | 78% |
| Tobacco-free campus | 92% |
| 24-hour nursing “help line” | 42% |
| Employee Assistance Program (EAP) | 93% |
| Wellness newsletter | 63% |
| Other program or benefit | 49% |
Here is a list of health care providers who are currently offering a comprehensive wellness program using the WellSteps platform:
Baptist Health
Church Health Center
Cleveland Chiropractic College/ Cleveland University – Kansas City
Community Hospital – McCook Nebraska
E4 Health Inc.
Emerus Holdings Inc
Fort Defiance Indian Hospital Board, Inc. (FDIHB)
Illinois Health and Hospital Association (IHA)
Lake Charles Memorial Health System
Mary Lanning Memorial HealthCare
And here is what the results of these wellness programs look like.
8. Hospitals are a Convenient and Easy Place to Focus on Prevention and Early Detection
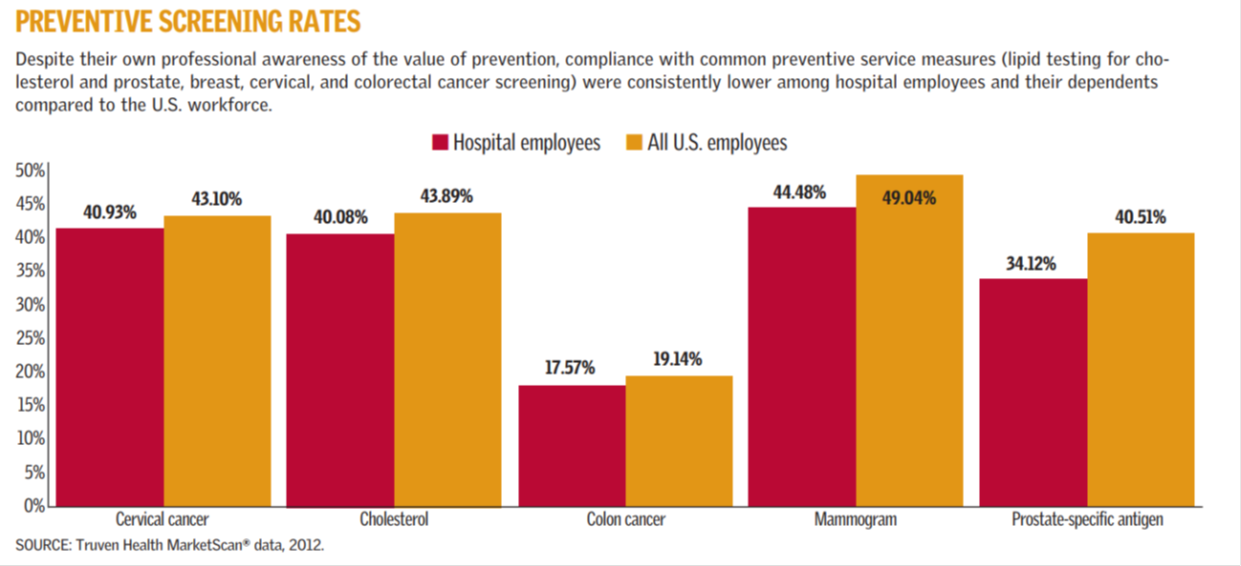
Unlike most worksites, hospitals, clinics, and healthcare facilities are the perfect places to promote the prevention and early detection of chronic diseases. Healthcare facilities are in the business of screening for cancers and giving injections. That’s why hospital wellness programs for employees are the perfect place to offer flu shots. These programs are also ideal for promoting early detection screenings such as mammography, colonoscopy, and other preventative screenings.
To get the most out of a wellness program every employee ought to have their blood screened at least once. Healthcare facilities are the perfect places to analyze blood samples because that’s what they do. A wellness program within a hospital setting could easily and affordably offer their employees biometric screenings. Hospitals are the perfect place to screen for elevated blood lipids, glucose, and blood pressure. Screening and gathering blood is actually the easy part. The hard part is convincing people to do something once they have identified elevated health risks.
Here’s a great article on exactly how to do the best biometric screenings.
You would think that because hospitals and other healthcare settings are the perfect place for healthcare workers to get screened that many of them would get screened. Surprisingly, that does not appear to be the case. A recent survey showed that health care workers and their dependents are actually not as compliant with common preventative screenings for cancer or for lipids when compared to other workers.
A great wellness program for hospitals should take full advantage of all screening resources that are available. They should also do a better job of communicating why employees should get screened.
9. Employee Wellness Programs are a Successful and Proven Business Strategy
Think of the different benefits employers typically offer. For example, these could include a retirement or pension plan, healthcare, paid time off, or maternity leave. These are designed to help your organization recruit and maintain qualified employees. Yet there are no studies or statistics that show that offering these benefits as any measurable effect on it worksite’s ability to recruit or maintain workers. We do them because we believe they are important.
These things are actually very hard to study; while we have a feeling they do make a difference in our ability to attract good workers, there is no science to back any of this up.
Now, in contrast, consider your hospital wellness program. Unlike all the other benefits your worksite offers, wellness programs have been studied for decades. There are hundreds and hundreds of rigorous scientific evaluations of the impact of wellness programs. in short, we are blessed to have mountains of workplace wellness statistics. There is more research on the impact of wellness programs than anything else your company does. Granted, the research is not perfect—no research ever is.
But after decades of scientists evaluating programs, we have an enormous amount of very solid statistical evidence that show the benefits of having a wellness program. I personally have published 75 research papers on the impact of worksite wellness programs. And I am just one of hundreds of scientists in the field.
Frequently Asked Questions
At WellSteps we believe in taking a comprehensive approach to health. There are seven main categories that all successful hospital wellness programs should know.
1. Physical – This is what comes to mind most often when people think of wellness. Physical health includes; getting plenty of sleep, proper nutrition and a healthy amount of physical activity.
2. Intellectual – This can also be described as personal growth. It is important for employees to create, learn new skills, and face new challenges.
3. Emotional – An emotionally healthy employee has the tools to understand and control their emotions. They are resilient, positive, and confident.
4. Social – It is important for employees to be able to have positive interactions with their community and to strengthen their personal relationships.
5. Occupational – Occupational health is achieved when an employee is happy with their job and the work life balance that it provides them.
6. Spiritual – You do not need to be religious to feel the benefits of a spiritually healthy lifestyle. What you do need is an understanding that life is meaningful. This can be found in a higher purpose, morals, etc.
7. Financial – This is when an employee feels at peace and confident with their current and future finances.
To learn more about how to define wellness, check out this blog post.
Earlier in this article, it states that you must have staff to administer the program, effective behavior change interventions/activities, and a web-based data platform on which to administer, communicate, and evaluate the program. A hospital wellness program should have activities that focus on the main health issues of the staff. This may differ from hospital to hospital. However, we know that obesity, lack of exercise, stress, and nutrition are common areas of concern for healthcare workers.
One of the most important indicators for success is senior leader support. So, the first step is to make sure you have a senior leader on board that will actively participate in the wellness program. We also recommend creating a wellness committee to give employees a voice and help make decisions. Next, you will need to assess the worksite health culture and employee behaviors. Use this information to create wellness goals and know your focus areas. You can do this with the help of a vendor or on your own.
Hospital wellness programs support employees who experience higher stress, emotional load, shift changes, and unpredictable schedules. Wellness is essential for hospitals because caregiver well-being directly affects patient outcomes.
Hospitals often see reduced turnover, better morale, lower injuries, improved teamwork, and fewer fatigue-related errors. These outcomes make hospital wellness programs a high-ROI investment.
With rotating shifts, healthcare employees must participate on their own schedule. Digital platforms ensure hospital wellness programs are available day or night.
Tools like WellSteps Custom Challenges, MyTracker, and Rewards simplify participation and tracking across multiple shifts—essential for large hospital wellness programs.
Burnout is the #1 threat to hospital retention. Effective hospital wellness programs integrate rest breaks, mental health support, hydration reminders, and sleep-focused challenges to rebuild resilience for clinical staff.

Hi Steve,
Nice article on 9 Reasons Hospital Wellness Program Are a Smart Business Strategy. Say, I’m not sure if you are interested or not but I would be glad to send you a ten-year program evaluation that Larry Chapman MPH and I did when I was the Wellness Administrator at a hospital beginning in 1990. The internal program was featured in many national publications. Reading your article brings back memories and also validates just how far ahead we were from the rest of the industry when it came to hospital wellness.
Ironically, we had both an internal and external wellness and prevention division and we very actively involved in providing wellness and prevention services to employers, beginning in 1988.
Anyway, I thought you might want to see what we did.
Best wishes!
Ron
Ron,
Nice to hear from you again. Is it something we can share with others? If so, perhaps we could post it the comments section for others to see.
Steve
Thanks Steve!
The actual program evaluation we did is pretty detailed, is fairly technical and probably wouldn’t make sense to be posted but there is a pretty detailed and descriptive case study that WELCOA did on the program. If you think that would work let me know.
Here is the link: http://www.ndworksitewellness.org/docs/step4-designing-wellness-incentive-part2.pdf
Comments are closed.